ADHD Diagnosis & Treatment for Children in Richardson, TX — Dr. John R. Porter’s Approach
If you’re reading this, chances are something has been nagging at you. Maybe a teacher mentioned your child has trouble staying focused. Maybe homework has become a nightly battle that leaves the whole family exhausted. Maybe you’ve noticed that your child seems to struggle with things that come easily to their peers — and you’re wondering whether it’s ADHD or just a phase.
You’re not alone. ADHD is one of the most common neurodevelopmental conditions in children, and it’s one of the conditions Dr. John R. Porter evaluates and manages most frequently at his Richardson practice. But a Google search can leave you with more anxiety than answers — conflicting opinions, worst-case scenarios, and generic advice that doesn’t tell you what would actually happen if you picked up the phone and made an appointment.
That’s why Dr. Porter put this guide together. It walks you through exactly how he approaches ADHD — from the moment a parent raises a concern, through evaluation, diagnosis, treatment, and long-term care.
ADHD care is one part of the comprehensive child healthcare Dr. Porter provides at his Richardson practice — a philosophy built on knowing each child as a whole person, not just a single diagnosis. No vague overviews. No copy-pasted medical jargon. Just a clear picture of what the process looks like in our office so you can make an informed decision for your child.
This guide is for families in Richardson, Plano, Garland, Allen, Murphy, and across the North Dallas area. Whether your child is four or fourteen, whether you’re just starting to wonder or you’ve already received a diagnosis elsewhere and want a second opinion, this page is here to help.
Recognizing ADHD in Your Child
What ADHD actually is — beyond the stereotypes
ADHD — Attention Deficit Hyperactivity Disorder — is a neurodevelopmental condition that affects how a child’s brain manages attention, impulse control, and activity level. It’s not a discipline problem. It’s not caused by bad parenting, too much sugar, or too many screens. It’s a real, well-researched medical condition rooted in how the brain develops and regulates itself.
There are three presentations of ADHD, and understanding which one your child fits can make a real difference in how it’s managed.

The first is the inattentive presentation. These are the kids who seem to daydream constantly, lose their belongings, forget instructions the moment you give them, and struggle to finish tasks — even ones they enjoy. They’re often quiet and compliant, which is why this type frequently goes undiagnosed, especially in girls.
The second is the hyperactive-impulsive presentation. This is closer to the classic image most people have of ADHD — the child who can’t sit still, blurts out answers, interrupts conversations, and seems to run on a motor that never shuts off.
The third is the combined presentation, which is the most common. These children show significant signs of both inattention and hyperactivity-impulsivity.
It’s worth saying what ADHD is not. Every child loses focus sometimes. Every child acts impulsively sometimes. ADHD is different because the symptoms are persistent, show up in more than one setting (home and school, not just one), and meaningfully interfere with a child’s ability to function at the level expected for their age.
How ADHD shows up at different ages
One thing that surprises many parents is how much ADHD changes as a child grows.
In toddlers and preschoolers, it can be especially hard to tell the difference between ADHD and normal developmental behavior. Most three-year-olds are impulsive. Most four-year-olds have trouble sitting still. But some children stand out — they’re significantly more active, more intense, or more disruptive than their peers in ways that teachers and caregivers notice consistently. They may have trouble playing with other children, following simple routines, or transitioning between activities without major meltdowns. At this age, Dr. Porter takes a careful, watchful approach. A diagnosis is possible but requires clear evidence that the behavior goes beyond what’s typical for the age.
In elementary school-age children, ADHD becomes much more visible because school demands things that ADHD makes hard — sitting still, listening to instructions, completing work independently, and organizing materials. This is the age when most families first raise concerns. Teachers may report that a child can’t stay on task, calls out in class, is constantly fidgeting, or seems bright but isn’t performing to potential. Richardson ISD, Plano ISD, and Garland ISD schools often bring up these observations during parent-teacher conferences, and that feedback is an important piece of the evaluation process.
In adolescents, the picture shifts again — and these changes are often first identified during a routine adolescent physical exam, where Dr. Porter screens for attention, mood, and executive function concerns alongside the standard wellness evaluation. What comes to the forefront are challenges with executive function: planning ahead, managing time, keeping track of assignments, staying motivated on long-term projects. Social and emotional challenges also grow. Teens with ADHD may struggle with friendships, be more prone to emotional outbursts, or develop anxiety or low self-esteem as they become more aware of how they compared to peers. Some teens are diagnosed for the first time during this stage because the demands of middle school or high school finally exceed their ability to compensate.
When to bring it up with your pediatrician
There’s no single sign that tells you it’s time to bring up ADHD. But there are patterns worth paying attention to.
If you’re hearing the same concerns from more than one source — a teacher and a coach, a grandparent and a tutor — that consistency is meaningful. If your child is struggling in school despite clearly being capable, that gap between potential and performance is one of the most common reasons families come in. If everyday tasks like getting dressed in the morning, following a two-step direction, or sitting through dinner have become ongoing battles, it’s worth exploring.
You don’t need to be certain. You don’t need to have a checklist filled out. You just need to have the conversation. For many families, a routine pediatric physical exam is where that conversation begins — Dr. Porter uses these visits to screen for developmental and behavioral concerns, including early signs of ADHD, even before a parent raises the question.
When you call our Richardson office at (972) 235-6911 to schedule, it helps to have a few things ready: specific examples of the behaviors you’ve noticed, any feedback you’ve received from teachers or school staff, and a general sense of how long the concerns have been present. But even if you don’t have any of that organized yet, that’s okay — Dr. Porter will walk you through it.
The Diagnostic Journey at Our Richardson Office
What your first visit looks like
The first visit is a conversation, not a test. Dr. Porter isn’t going to hand you a form, glance at the results, and give you a diagnosis in twenty minutes. That’s not how responsible ADHD evaluation works, and it’s not how he practices.
When you arrive at our office at 1112 N Floyd Rd #10 in Richardson, the visit starts with Dr. Porter sitting down with you — and often with your child, depending on their age — to understand what’s been going on. He’ll ask open-ended questions.
- What does a typical school day look like?
- What does homework time look like?
- How does your child handle transitions, frustration, social situations?
- What are they great at? What feels like a constant fight?
He’ll want to hear the full story, not just the problematic moments. Kids with ADHD are not struggling in every area of their lives. Many are creative, funny, deeply empathetic, and capable of intense focus on things that interest them.
Understanding the whole child — not just the symptoms — is essential to making the right call and building a plan that actually works for your family.
Dr. Porter will also dig into your child’s developmental history.
- When did they hit milestones?
- Were there any complications during pregnancy or birth?
- Is there a family history of ADHD, anxiety, depression, or learning differences?
These details matter because ADHD has a strong genetic component, and the developmental timeline helps distinguish ADHD from other conditions that can look similar on the surface.One thing Dr. Porter will make clear at this first visit: a diagnosis might not happen today.
For some children the picture is straightforward, but for many, a responsible evaluation takes more than one appointment. He’d rather take the time to get it right than rush to a label that may not fit.
How long the process takes
Most families want to know upfront: how long is this going to take? The honest answer is that it varies, but Dr. Porter’s typical evaluation process spans two to three visits over a few weeks.
The first visit is the detailed conversation described above, where Dr. Porter gathers history and begins forming a clinical picture. At that visit, rating scale forms go home with you and are sent to your child’s teacher. There’s usually a waiting period while those come back — sometimes a few days, sometimes a couple of weeks depending on how quickly the school responds.
The second visit is where Dr. Porter reviews the completed rating scales alongside his own observations and the history you’ve provided. In many cases, this is where a diagnosis can be made with confidence. In other cases — particularly when the symptoms are mild, when there’s overlap with anxiety or a learning disability, or when the parent and teacher reports tell very different stories — Dr. Porter may recommend additional evaluation before drawing a conclusion. That might mean a follow-up visit with more targeted questions, or it might mean a referral for neuropsychological testing with a specialist in the Richardson or North Dallas area to get a more detailed cognitive profile.
Dr. Porter doesn’t rush this. A premature diagnosis can lead to unnecessary medication. A missed diagnosis can lead to years of avoidable struggle. Taking a few extra weeks to be thorough is always worth it, and he’ll explain his reasoning at every step so you’re never left wondering what’s happening or why.
Delivering the diagnosis
When Dr. Porter is confident in the diagnosis, he doesn’t deliver it in passing at the end of a rushed visit. He sits down with parents — and with the child when age-appropriate — and walks through the findings in plain language.
He’ll explain what the rating scales showed, what his clinical observations revealed, and how all of that lines up with the diagnostic criteria. He’ll tell you which presentation of ADHD your child fits — inattentive, hyperactive-impulsive, or combined — and what that means in practical terms for your child’s daily life.
Just as important as what the diagnosis means is what it doesn’t mean. It doesn’t mean your child is broken. It doesn’t mean they’ll never succeed in school. It doesn’t mean medication is inevitable. It means their brain works differently in specific, well-understood ways, and now that you know that, you can build a support system around it instead of fighting against it.
At this visit, Dr. Porter will outline an initial plan. For some families, that starts with behavioral strategies and school accommodations. For others, the symptoms are severe enough that medication makes sense from the beginning. For many, it’s a combination. He’ll explain his reasoning, give you space to ask questions, and make sure you leave the office with a clear understanding of what happens next — not just a diagnosis and a prescription.
If the evaluation determines that your child does not have ADHD, that’s valuable information too. Dr. Porter will discuss what he thinks is actually going on and what the appropriate next steps are — whether that’s monitoring, further testing, or a referral to another specialist. A thorough evaluation is never wasted, even when the answer isn’t what you expected.
Treatment — Dr. Porter’s Approach
Starting with the full picture
There’s a misconception that an ADHD diagnosis automatically means a prescription. In Dr. Porter’s practice, that’s not how it works. Medication may be part of the plan — and for many children, it’s an important part — but it’s never the entire plan, and it’s never the automatic first step for every child who walks through the door.
Dr. Porter builds a treatment approach around your specific child. Not ADHD in the abstract, but your child — their age, their symptom severity, how much their daily life is being affected, what’s happening at school, what your family’s preferences and concerns are, and what has or hasn’t been tried before.
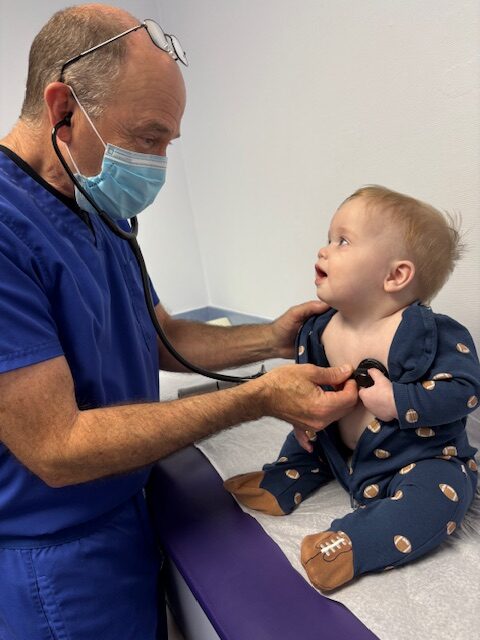
A six-year-old who’s struggling with classroom behavior but doing okay academically is a very different situation than a twelve-year-old who’s failing three classes and developing anxiety about school. A family that’s open to trying medication right away is in a different starting place than a family that wants to exhaust every other option first. Both are valid. Dr. Porter’s job is to lay out the options clearly, give you his honest clinical recommendation, and then build the plan together with you — not hand it down to you.
His general philosophy leans toward starting with the least intensive intervention that’s likely to make a meaningful difference. For mild cases, especially in younger children, that often means behavioral strategies and school supports first. For moderate to severe cases, particularly when a child is falling significantly behind or developing emotional problems as a consequence of untreated ADHD, he’ll recommend medication earlier in the process — not because it’s the easy answer, but because waiting too long has its own costs.
Behavioral strategies and non-medication interventions
Behavioral strategies aren’t a consolation prize for families who don’t want medication. They’re a foundational part of ADHD management regardless of whether medication is also in the picture. Medication can improve a child’s ability to focus and control impulses, but it doesn’t teach them how to organize a backpack, break a project into steps, or manage frustration when something doesn’t go their way. That’s where behavioral strategies come in.
At the household level, Dr. Porter works with families on building structure and predictability into daily routines. Children with ADHD do better when expectations are clear, consistent, and external — meaning they don’t have to rely on their own memory and internal motivation to get through the day. That might look like a visual checklist for the morning routine, a consistent homework time and location with minimal distractions, or a clear and calm system of consequences and rewards that’s applied the same way every day. None of this is groundbreaking. But the consistency is what makes it work, and Dr. Porter helps families figure out what’s realistic for their specific household rather than handing over a generic handout.
For younger children especially, parent training programs can be remarkably effective. These are structured programs — often run by psychologists or behavioral therapists — that teach parents specific techniques for managing ADHD-related behavior. Giving effective commands, reinforcing positive behavior, reducing attention to minor misbehavior, and handling defiance without escalation. Dr. Porter regularly refers families to behavioral health providers in the Richardson and North Dallas area who run these programs, and he can help you find the right fit based on your child’s age and your family’s needs.
For some children — particularly those with milder symptoms, those under six, or those whose ADHD is primarily causing problems in one setting — behavioral strategies and school supports may be all that’s needed, at least initially. Dr. Porter will set a clear timeline for reassessment so that if things aren’t improving enough, the conversation about additional interventions happens promptly rather than dragging on while your child continues to struggle.
Medication — how we approach the decision
When behavioral strategies alone aren’t producing enough improvement, or when the severity of symptoms makes it clear from the start that behavioral approaches by themselves won’t be sufficient, Dr. Porter will talk with you about medication. This is a conversation, not a directive. He’ll explain why he’s recommending it, what the realistic benefits are, what the side effects can look like, and what the process of finding the right medication and dose involves. He wants you to make this decision with your eyes open, not out of desperation or pressure.
The two main categories of ADHD medication are stimulants and non-stimulants, and understanding the difference matters.
Stimulant medications — the methylphenidate family (which includes brand names like Ritalin, Concerta, and Focalin) and the amphetamine family (which includes Adderall, Vyvanse, and Dyanavel) — are the first-line treatment for ADHD in children. That’s not because the medical community defaulted to the easy option. It’s because decades of research have consistently shown that stimulants are the most effective medication for ADHD symptoms in the majority of children. They work by increasing dopamine and norepinephrine activity in the brain, which improves focus, impulse control, and the ability to regulate behavior.
Dr. Porter typically starts with a low dose of a stimulant medication and increases gradually. This is called titration, and it’s how he finds the dose that provides the most benefit with the fewest side effects. He’ll choose between short-acting and long-acting formulations based on your child’s age, school schedule, and how their symptoms are distributed throughout the day. A child who only struggles during school hours has different needs than a child whose symptoms affect everything from breakfast to bedtime.
Non-stimulant medications — such as atomoxetine (Strattera), guanfacine (Intuniv), and clonidine (Kapvay) — are an alternative for children who don’t respond well to stimulants, who experience side effects that can’t be managed with dose adjustments, or who have co-occurring conditions like anxiety or tics that make stimulants a less ideal choice. They work through different brain pathways, tend to have a slower onset of action, and have a different side effect profile. Dr. Porter will explain when and why a non-stimulant might be the better starting point for your child.
One thing he’s transparent about: finding the right medication and the right dose is a process. It’s common to need adjustments in the first weeks or months. That doesn’t mean medication isn’t working or that the diagnosis is wrong. It means your child’s brain is unique, and the fine-tuning takes time and close follow-up.
Ongoing medication management
Starting a medication is not the finish line. It’s the beginning of an ongoing partnership between your family and Dr. Porter’s office.
In the early weeks after starting or changing a medication, follow-up is frequent. Dr. Porter typically wants to hear from you within the first one to two weeks — sometimes with an office visit, sometimes with a phone or portal check-in — to find out how things are going. Is your child focusing better? Are there side effects? How’s their appetite? Are they sleeping? What’s the teacher reporting? This early feedback is how he decides whether the current dose is right, needs to go up, or needs to be reconsidered entirely.
Once a stable, effective dose is established, visits spread out — but they don’t stop. Dr. Porter sees children on ADHD medication regularly, typically every three to four months. At these visits, he’s checking multiple things. Growth — because stimulant medications can sometimes suppress appetite and affect weight gain. Sleep — because many ADHD medications can interfere with falling asleep if the timing or dose isn’t right. Mood — because some children develop irritability, emotional flatness, or increased anxiety on certain medications. Academic and behavioral functioning — because the whole point of treatment is real-world improvement, not just a controlled substance refill.
He also monitors for the need to adjust. Children grow. Their brain chemistry changes. The demands placed on them increase as they move from elementary school to middle school to high school. A dose that worked perfectly in third grade may not be adequate in sixth grade — not because the medication stopped working, but because the environment changed. Dr. Porter adjusts proactively, based on data and conversation, rather than waiting for a crisis to signal that something needs to change.
And he’s honest with families about medication breaks. Some parents ask about taking their child off medication during weekends or summer. In some cases, this makes sense — it can give you useful information about how your child functions without medication, and it can help with appetite or growth concerns. In other cases, it’s counterproductive — if your child’s ADHD significantly affects their social life, their self-esteem, or their ability to function at home, a medication break doesn’t give them a break from ADHD. It just removes the support. Dr. Porter discusses this on a case-by-case basis rather than applying a blanket policy.
School and Daily Life in North Texas
Working with your child’s school
An ADHD diagnosis doesn’t just change what happens in Dr. Porter’s office. It changes what’s possible at school — but only if you know how to access the right support. Many parents in the Richardson area don’t realize how much their child is entitled to, or how the process of getting that support actually works in local districts. This section is meant to close that gap.
There are two main avenues for school-based ADHD support: a 504 plan and an IEP. They sound similar but they’re different in important ways, and which one your child qualifies for — and which one they actually need — depends on their specific situation.
A 504 plan is the more common path for children with ADHD. It falls under Section 504 of the Rehabilitation Act, which is a federal civil rights law. It requires the school to provide reasonable accommodations that give your child equal access to learning. The key word is accommodations — changes to how your child is taught and tested, not changes to what they’re taught. Common 504 accommodations for ADHD include preferential seating near the teacher and away from distractions, extended time on tests and major assignments, permission to take breaks during long tasks, reduced homework volume when the standard load is excessive for the child’s capacity, written instructions instead of verbal-only directions, and check-ins with a teacher or counselor during the day.
A 504 plan is relatively straightforward to put in place. In Richardson ISD, Plano ISD, and Garland ISD, the process typically starts with a parent request — verbal or written — to the school counselor or 504 coordinator. The school convenes a small committee, reviews documentation (which Dr. Porter’s office provides), and determines eligibility. If your child qualifies, the plan is written and shared with every teacher who works with your child. The whole process often takes a few weeks, though timelines can vary by campus and time of year.
An IEP — Individualized Education Program — is a different and more intensive level of support. It falls under the Individuals with Disabilities Education Act (IDEA) and provides not just accommodations but specialized instruction and services. An IEP is appropriate when ADHD is significantly impacting your child’s ability to make academic progress even with accommodations — or when ADHD coexists with a learning disability that requires specialized teaching methods.
The IEP process is more formal. It involves a full evaluation by the school district’s special education team, which includes educational testing and often a psychological assessment. Parents have the right to request this evaluation in writing, and the district is required to respond within a set timeline. In Texas, the school has 15 school days to decide whether to evaluate after receiving a written request, and then 45 school days to complete the evaluation once consent is given. Dr. Porter’s office can provide clinical documentation to support the request, and he’s familiar with how special education departments in Richardson ISD, Plano ISD, and Garland ISD handle these cases.
Which path is right for your child? In Dr. Porter’s experience, most children with ADHD are well-served by a solid 504 plan, especially when the family, school, and medical team are communicating effectively. An IEP becomes necessary when ADHD alone or in combination with a learning disability is creating a gap that accommodations alone can’t close. Dr. Porter will help you think through which route makes sense and will provide whatever documentation the school needs to move the process forward.
One thing he encourages every parent to know: you are a member of the team. You have the right to attend every meeting, to ask questions, to disagree, and to request changes. The school is your partner, not the gatekeeper. If you feel like you’re not being heard or that the plan isn’t working, Dr. Porter’s office can help you navigate that — including writing letters, providing updated clinical information, or recommending that you request a meeting to revise the plan.
Supporting your child at home
School is where ADHD often gets the most attention, but home is where your child lives most of their life — and where some of the most important support happens.
The single most impactful thing Dr. Porter recommends to families is structure that doesn’t depend on your child’s memory. Children with ADHD aren’t forgetting their homework or losing their jacket because they don’t care. Their working memory — the mental system that holds information in mind while they act on it — is often significantly weaker than their peers’. Telling them three things to do and expecting them to remember all three is setting them up to fail. Giving them a visible, predictable system makes it possible for them to succeed.
That system looks different in every family, but the core principles are the same. Routines should be consistent — the same morning sequence, the same after-school rhythm, the same bedtime process — so that the steps become automatic over time instead of requiring a fresh act of willpower every day. Instructions should be short, specific, and one at a time. “Go clean your room” is overwhelming. “Put your dirty clothes in the hamper” is actionable. Visual cues — a whiteboard checklist by the door, a color-coded calendar, a bin where shoes and backpack always go — remove the burden from memory and put it in the environment.
Homework is where many families hit their breaking point. Dr. Porter’s advice is to create a homework environment that minimizes competition for your child’s attention. A consistent time, a consistent place, no television or phone nearby, and a parent who’s available but not hovering. Break assignments into smaller chunks with short breaks in between. If homework is consistently taking far longer than it should — more than ten minutes per grade level is a common benchmark — that’s information worth sharing with the teacher and with Dr. Porter, because it may signal a need to adjust accommodations or treatment.
And then there’s the piece that doesn’t show up on any checklist: your child’s self-image. Children with ADHD hear more correction, more redirection, and more frustration directed at them than their peers. Over time, that accumulates. They start to internalize it. They become the kid who’s always in trouble, always forgetting, always behind. One of the most powerful things you can do at home is make sure your child knows that ADHD is one part of who they are — not the defining part. Catch them doing things well. Name their strengths out loud. Make sure the ratio of positive to corrective interactions tilts heavily toward the positive, even on hard days. Dr. Porter raises this with families not because it’s soft advice, but because a child’s belief about their own capability shapes everything — their motivation, their willingness to try, their resilience when things go wrong.
Social and emotional challenges
ADHD doesn’t stay in the classroom. It follows your child to the playground, to birthday parties, to the lunch table, and to the group chat. The social and emotional side of ADHD is often the part that weighs heaviest on families — and the part that gets the least attention.
Children with ADHD frequently struggle with friendships. The impulsive child interrupts, talks over others, and has trouble waiting their turn in games. The inattentive child zones out during conversation and misses social cues. Both types may struggle to read the room — to notice when someone is annoyed, bored, or upset — because the same executive function deficits that affect academics also affect social awareness. The result is that many children with ADHD experience peer rejection, and they feel it deeply even if they can’t always articulate it.
There’s a concept in the ADHD research called rejection sensitive dysphoria — an intense emotional reaction to perceived criticism or rejection. Not every child with ADHD experiences it, but many do, and it can look like extreme upset over minor social slights, rage or tears in response to constructive feedback, or avoidance of situations where failure or rejection is possible. If your child seems to overreact to things that seem small to you, this may be part of the picture.
Dr. Porter talks with families about these dynamics because they affect treatment decisions. A child whose ADHD is primarily causing social and emotional suffering — even if their grades are fine — may benefit from medication, therapy, or both. Social skills groups, which are available through several practices in the Richardson and Plano area, can give children a structured, low-pressure environment to practice the skills that don’t come naturally. Individual therapy — particularly cognitive behavioral therapy — can help older children and teens develop strategies for managing emotional reactions, building self-awareness, and handling conflict.
When Dr. Porter sees a child whose emotional challenges are significant — persistent sadness, intense anxiety, social withdrawal, or escalating behavioral problems — he doesn’t treat it as a footnote to the ADHD diagnosis. He addresses it directly, either within the management plan or by connecting the family with a therapist or psychologist who can provide the level of support the child needs.
Coordinating Care Across North Dallas Providers
When Dr. Porter refers to other specialists
Dr. Porter manages the majority of ADHD cases in his practice from start to finish — evaluation, diagnosis, medication management, school coordination, and ongoing follow-up. That’s by design. Pediatricians who know a child and family well over time are often in the best position to manage ADHD, because they see the full picture — not just the ADHD, but the ear infections, the growth patterns, the anxiety that showed up in fourth grade, the family stress that flared up during a divorce. Context matters, and Dr. Porter has it.
But there are situations where a child needs more than what a pediatric office can provide, and Dr. Porter is straightforward about recognizing those moments rather than pushing past them.
Pediatric psychiatry becomes part of the conversation when the medication picture is complicated. That might mean a child who has tried multiple medications without adequate improvement. It might mean ADHD that coexists with significant anxiety, depression, or a mood disorder, where the interaction between medications requires specialized expertise. Or it might mean a child whose behavioral challenges are severe enough to need a level of psychiatric monitoring that goes beyond what a routine pediatric visit can accommodate. Dr. Porter works with pediatric psychiatrists in the Richardson, Plano, and greater North Dallas area and can refer your family to someone he trusts when the situation calls for it.
Neuropsychological testing is something Dr. Porter recommends when the diagnostic picture is murky. If a child isn’t responding to ADHD treatment the way he’d expect, or if there are signs that a learning disability, processing disorder, or intellectual giftedness is layered on top of or mimicking ADHD, a neuropsychological evaluation can sort that out. These evaluations are comprehensive — typically four to eight hours of testing across multiple cognitive domains — and they produce a detailed profile of how a child’s brain processes information. The results don’t just clarify the diagnosis. They generate specific, actionable recommendations for school and home. Several neuropsychology practices in the North Dallas area provide this testing, and Dr. Porter can guide you to one that matches your child’s needs and your insurance situation.
Therapy is not something every child with ADHD needs, but many benefit from it. Dr. Porter refers to therapists for several reasons. Cognitive behavioral therapy can help older children and teens develop practical coping strategies — managing frustration, organizing their thinking, handling social conflict, and building habits that compensate for executive function weaknesses. Behavioral therapy for younger children often works through the parents, teaching specific techniques for managing behavior at home. Family therapy may be appropriate when ADHD is creating significant stress between parents, between siblings, or between a parent and child — when the household dynamic itself has become part of the problem and needs its own attention. Dr. Porter maintains relationships with behavioral health providers across the Richardson and North Dallas area and can match your family with the right type of therapist rather than sending you off with a generic list.
Developmental pediatrics is a less common referral but an important one. If a child’s presentation is unusually complex — ADHD alongside autism spectrum traits, significant developmental delays, or a pattern that doesn’t fit neatly into any single diagnosis — a developmental pediatrician can conduct a broader evaluation and help build a more comprehensive management plan. Children’s Health and UT Southwestern, both accessible from Richardson, have developmental pediatrics programs that Dr. Porter refers to when this level of assessment is warranted.
How we stay connected across providers
A referral from Dr. Porter’s office is not a handoff. It’s an expansion of the team, with Dr. Porter remaining at the center of your child’s care.
When he refers your child to a specialist, he sends the relevant clinical information — his notes, the rating scales, his diagnostic reasoning, and what’s been tried so far. He doesn’t send you to a psychiatrist or neuropsychologist and expect them to start from scratch. And when the specialist sends findings back, Dr. Porter reviews them, integrates them into your child’s care plan, and discusses the implications with you at your next visit.
This matters more than most families realize. When a child sees multiple providers who don’t communicate, things fall through the cracks. A psychiatrist adjusts a medication, but the pediatrician doesn’t know about it. A neuropsychologist recommends specific school accommodations, but no one follows up to make sure the school implements them. A therapist identifies a new concern, but it never makes it back to the medical team. Dr. Porter’s practice actively works to prevent those gaps.
He coordinates not just with the specialists he refers to, but with your child’s school. If a neuropsychological evaluation produces school recommendations, Dr. Porter’s office can help translate those into language that supports a 504 plan or IEP request. If a psychiatrist makes a medication change, Dr. Porter keeps track of it and monitors for effects at subsequent visits. The goal is that no matter how many providers are involved, your family has one home base — Dr. Porter’s office at 1112 N Floyd Rd in Richardson — where the full picture lives and someone is paying attention to all of it.
There are things parents can do to help keep this coordination tight. Bring reports and notes from other providers to your appointments with Dr. Porter, even if you think they’ve already been sent. Mention any changes — new medication, new therapist, new concerns raised at school — even if they seem minor. Ask questions when you’re unsure how one provider’s recommendations connect to another’s. The more information flowing into the shared picture, the better the care your child receives.
The Long-Term Outlook
What research says about ADHD across the lifespan
Parents often ask Dr. Porter what the future holds for a child with ADHD. It’s an understandable question, and the honest answer is more encouraging than most people expect.
ADHD is a real, persistent condition — but it is not a ceiling on what your child can achieve. The research is clear on this. Children with ADHD who receive appropriate diagnosis, consistent treatment, and strong support systems go on to succeed in school, in careers, and in relationships. They become doctors, engineers, teachers, business owners, artists, and athletes. ADHD shapes how they get there, but it doesn’t determine where they end up.
That said, the research is equally clear that untreated or poorly managed ADHD carries real risks over time. Children who never receive support are more likely to struggle academically, more likely to develop secondary anxiety or depression, more likely to have difficulty with peer relationships, and more likely to experience problems with self-esteem that follow them into adulthood. In adolescence, untreated ADHD is associated with higher rates of risky behavior, substance experimentation, and driving accidents — not because ADHD makes a child reckless by character, but because impulsivity without support is a vulnerability.
This is not meant to frighten you. It’s meant to reinforce something Dr. Porter believes deeply: early, thoughtful intervention matters. Not because your child is fragile, but because they deserve every advantage you can give them while their brain is still developing and their habits are still forming. The work you’re doing now — reading this guide, asking questions, considering an evaluation — is already part of that investment.
How Dr. Porter helps families plan for transitions
ADHD doesn’t stay the same as your child moves through different stages of life, and neither should the management plan. One of the things Dr. Porter pays close attention to is transitions — the moments when the demands on your child change significantly and the strategies that were working may need to change too.
The move from elementary to middle school is one of the most disruptive transitions for children with ADHD. In elementary school, your child typically has one teacher who knows them well, a structured day with clear routines, and a contained environment. In middle school, suddenly there are six or seven teachers, a locker to manage, a rotating schedule, long-term projects with distant deadlines, and a social landscape that’s dramatically more complex. Many children who were managing adequately in elementary school hit a wall in sixth or seventh grade — not because their ADHD got worse, but because the environment got harder. Dr. Porter works with families in the year leading up to this transition to prepare. That might mean adjusting medication, strengthening organizational systems, updating the 504 plan to reflect middle school demands, or connecting with the new school’s counseling team before the first day.
The move from middle school to high school brings another shift. Academic expectations intensify. Independence is expected. The social stakes feel higher. Driving enters the picture. For teens with ADHD, this stage often requires a recalibration — revisiting whether the current treatment plan is adequate, having direct conversations with the teen about their own role in managing their ADHD, and beginning to shift responsibility from parent-driven management to self-management with parental support. Dr. Porter begins this shift intentionally rather than waiting for it to happen by default.
This is also the stage where Dr. Porter’s adolescent physical exam becomes especially valuable — it provides a structured touchpoint to reassess ADHD management alongside the broader physical and emotional changes of the teenage years.
And then there’s the transition that many families don’t think about until it’s right around the corner: leaving for college or adulthood. A child who has been managed by their parents and their pediatrician for a decade suddenly needs to manage their own medication, their own appointments, their own schedule, and their own academic accommodations — often while living away from home for the first time. Dr. Porter starts preparing families for this transition well before it arrives. That includes helping the teen understand their own diagnosis and treatment history, teaching them how to communicate with future providers, ensuring they know how to request accommodations at the college level (which operates under different laws than K-12), and in some cases transitioning care to an adult provider who can continue what’s been built.
Building independence and self-advocacy skills over time
The long-term goal of ADHD management isn’t to create a child who’s perfectly managed by the adults around them. It’s to build a young person who understands their own brain, knows what helps them succeed, and can ask for what they need.
This doesn’t happen overnight. It’s a gradual process that Dr. Porter supports across years of care.
For younger children, self-advocacy starts small. It might mean a child learning to tell their teacher “I need to move around for a minute” instead of acting out. Or recognizing that they’re getting frustrated and using a strategy they’ve practiced instead of melting down. These are seeds. They don’t look like much at the time, but they grow.

For older children and teens, self-advocacy becomes more sophisticated. It means understanding what ADHD is and how it affects them personally — not as a label or an excuse, but as real self-knowledge. It means knowing that they focus better with background music, or that they need to break projects into pieces, or that they should sit in the front of the classroom, or that they process information better when they can take notes a certain way. It means being able to walk into a teacher’s office or a college disability services center and explain what they need without shame or apology.
Dr. Porter models this in his own interactions with his patients. As children get older, he increasingly talks directly to them during visits — not just to their parents. He asks them what’s working and what isn’t. He explains why he’s recommending a medication change or a new strategy. He treats them as partners in their own care, because that’s what they need to become.
Why ongoing care matters even when things are going well
There’s a natural temptation, once things stabilize, to step back from regular appointments. Your child is doing well in school. The medication seems to be working. The behavioral strategies are in place. Why keep coming in?
Dr. Porter understands the instinct, but he encourages families to maintain regular follow-up even during the good stretches — and here’s why.
ADHD management is not a problem you solve once. It’s an ongoing calibration. Your child’s brain is developing. Their body is growing, which affects medication dosing. Their environment is changing — new teachers, new schools, new social dynamics, new academic demands. A plan that’s working perfectly in September may need adjustment by February. Regular check-ins allow Dr. Porter to catch emerging issues early, fine-tune the approach proactively, and stay connected with how your child is actually doing rather than relying on a snapshot from months ago.
These visits also serve as a touchpoint for the less visible aspects of ADHD. A child might be doing fine academically but quietly developing anxiety. A teen might be getting good grades but staying up until midnight to do it. A medication might be technically effective but causing subtle side effects that your child hasn’t mentioned because they’ve gotten used to them. The routine visit is where these things surface, and where they can be addressed before they become bigger problems.
Staying connected with care also sends a message to your child: this matters, you matter, and we’re paying attention. That consistency is its own form of support.
If you’ve read this far, it says something about you as a parent. You’re taking the time to understand what your child is experiencing, what the options are, and what thoughtful, individualized care actually looks like. That matters more than you might realize.
Dr. Porter’s approach to ADHD has never been about quick diagnoses or one-size-fits-all treatment plans. It’s about knowing your child, partnering with your family, and building a plan that evolves as your child grows. Whether your child is two visits into an evaluation or ten years into management, the commitment is the same: careful attention, honest communication, and a genuine investment in your child’s long-term success.
If you’re ready to schedule an ADHD evaluation, have questions about your child’s current treatment, or want a second opinion on an existing diagnosis, we’re here.
Common Questions From Richardson-Area Parents
Will my child be on medication forever?
Not necessarily, and this is one of the most common concerns Dr. Porter hears. ADHD is typically a lifelong condition — it doesn’t go away at a certain age — but that doesn’t automatically mean lifelong medication. Some children eventually develop coping strategies and executive function skills that allow them to manage well without medication, particularly if their symptoms are mild to moderate. Others find that medication remains helpful into adolescence and adulthood. Dr. Porter reassesses regularly. As your child grows, the question isn’t whether they’ll be on medication forever — it’s whether medication is still providing meaningful benefit right now. If there’s a point where it makes sense to try tapering off, he’ll discuss it with you and plan it carefully rather than abruptly stopping.
Does ADHD medication change my child’s personality?
This is a fear almost every parent has, and it deserves a direct answer. The right medication at the right dose should not turn your child into a different person. It should make them more able to do the things they already want to do — focus, complete tasks, control impulses, participate in conversations — without blunting the qualities that make them who they are.
That said, some children do experience emotional flatness, reduced spontaneity, or a subdued demeanor on certain medications or at doses that are too high. Dr. Porter watches for this actively, and he takes it seriously. If your child seems like a zombie, seems joyless, or seems to have lost their spark, that’s not an acceptable trade-off — it means the medication or the dose needs to change. He’ll adjust until the balance is right: meaningful symptom improvement with your child’s personality fully intact. And if you’re seeing something at home that concerns you, don’t wait for the next appointment. Call the office at (972) 235-6911 and let us know.
Is ADHD overdiagnosed?
This is a question Dr. Porter gets from parents who are skeptical, from parents who’ve just received a diagnosis they weren’t expecting, and from family members who think the child just needs more discipline. He addresses it head-on.
The research suggests a more nuanced picture than the headlines imply. In some populations and some settings, ADHD is probably overdiagnosed — particularly when diagnoses are made quickly, without standardized tools, and without gathering information from multiple sources. But in other populations, ADHD is significantly underdiagnosed — especially in girls, in children who present primarily with inattention rather than hyperactivity, and in communities where mental health evaluation carries stigma.
What Dr. Porter can tell you is how he guards against both errors in his own practice. He uses validated screening tools. He gathers input from parents and teachers. He rules out alternative explanations. He doesn’t diagnose in a single visit unless the evidence is overwhelming. And he doesn’t diagnose based on a gut feeling or a parent’s request — he diagnoses based on whether your child meets established clinical criteria across multiple settings. If your child has ADHD, he’ll tell you. If they don’t, he’ll tell you that too, and help you figure out what’s actually going on.
Can my child outgrow ADHD?
Some children do see a significant reduction in symptoms as they mature — particularly the hyperactive and impulsive symptoms, which tend to decrease with age more than the inattentive symptoms. By adulthood, a meaningful percentage of people who were diagnosed with ADHD as children no longer meet full diagnostic criteria.
But “outgrowing” ADHD isn’t something you can count on or plan around. Many children carry their symptoms into adulthood in some form. What typically changes is not the ADHD itself but the person’s ability to manage it — through learned strategies, environmental choices, and in some cases continued medication. Dr. Porter’s approach is to treat the child in front of him today, monitor over time, and celebrate progress whenever it comes rather than promising a specific outcome down the road.
What if the other parent disagrees about treatment?
This comes up more often than people might expect, and Dr. Porter handles it with care. Disagreements between parents about ADHD — whether it’s a real diagnosis, whether medication is appropriate, whether the school needs to be involved — are common and don’t make either parent wrong for having concerns.
When parents are not on the same page, Dr. Porter is willing to meet with both parents together to discuss the diagnosis, answer questions, and address specific fears. He finds that many disagreements stem from misinformation or fear rather than fundamental incompatibility, and a direct conversation with the treating physician can go a long way. He’s not there to take sides. He’s there to present the evidence clearly and help both parents make an informed decision that puts their child’s wellbeing first.
In situations involving divorced or separated parents, Dr. Porter is mindful of custody arrangements and decision-making authority. He works within whatever legal framework is in place and does his best to keep both parents informed and involved, because a child does best when the adults in their life are aligned — even if they don’t live in the same house.
How do I explain ADHD to my child?
This depends heavily on your child’s age and temperament, but Dr. Porter encourages parents not to avoid the conversation. Children who are struggling already know something is different about them. Giving it a name and an explanation — one that’s accurate and free of shame — is almost always better than letting them draw their own conclusions, which tend to be far worse. A six-year-old who’s told “your brain sometimes has a hard time putting on the brakes, and we’re going to help it” is better off than a six-year-old who’s decided “I’m the bad kid.”
For older children and teens, the conversation can be more detailed. Dr. Porter is happy to be part of it if that would help — explaining to your child directly, in age-appropriate language, what ADHD is, how it affects them specifically, and what the plan is to help. Some kids are relieved. Some are resistant. Some need time to process. All of those reactions are normal, and Dr. Porter can help you navigate the follow-up conversations at home.
Do you accept my insurance?
Insurance coverage and accepted plans can change, so rather than listing specific carriers here, the best thing to do is call our office directly at (972) 235-6911. Our front desk team can verify your coverage and let you know about any out-of-pocket costs before your first appointment. We want the financial side of care to be as clear and stress-free as the clinical side.
