Childhood Asthma Diagnosis & Treatment in Richardson, TX — Dr. John R. Porter’s Approach
If your child has a cough that never quite goes away — the one that lingers for weeks after every cold, that shows up at bedtime, that makes you pause every time they run across the yard — you’ve probably asked yourself whether something more is going on.
You’re right to wonder. A cough that keeps coming back, wheezing that shows up during exercise or cold weather, a child who seems to get “bronchitis” every few months — these aren’t always just bad luck with viruses. For many children, they’re early signs of asthma. And the difference between recognizing that pattern early and waiting years for a diagnosis can mean the difference between a child who thrives and a child who quietly struggles.
Asthma is one of the most common chronic conditions in children, and it’s one of the conditions Dr. John R. Porter manages most frequently at his Richardson practice. It’s also one of the most manageable — when it’s properly diagnosed, clearly explained, and carefully monitored over time. That’s what this guide is about. Not a textbook definition of asthma, but a clear, detailed walkthrough of how Dr. Porter actually approaches it: how he evaluates a child with breathing concerns, how he makes the diagnosis, how he builds a treatment plan with your family, and how he adjusts that plan as your child grows.
Asthma management is one part of the comprehensive pediatric health care services Dr. Porter provides at his Richardson office — a practice built on knowing each child as a whole person and partnering with families for the long haul.
This guide is for families in Richardson, Plano, Garland, Allen, Murphy, and across the North Dallas area. Whether your child has just started wheezing or has been living with asthma for years and you’re looking for a better approach, this page is here to help.
If at any point you’d like to schedule an evaluation, you can call our office at (972) 235-6911 or visit us at 1112 N Floyd Rd #10, Richardson, TX 75080.
Recognizing Asthma in Your Child
What asthma actually is — beyond “just wheezing”
Asthma is a chronic condition that affects the airways — the tubes that carry air in and out of your child’s lungs. In a child with asthma, three things happen inside those airways that make breathing harder than it should be. The lining of the airways becomes inflamed and swollen, which narrows the space air can move through. The muscles around the airways tighten, narrowing them even further. And the airways produce excess mucus, which clogs things up and triggers coughing.

What makes asthma different from a one-time wheeze during a bad cold is that these airways are chronically sensitive. They overreact to things that don’t bother most people — cold air, exercise, pollen, a viral infection, cigarette smoke, even strong emotions. When those triggers hit, the airways clamp down, and your child has what’s commonly called an asthma attack or flare-up.
But here’s the thing that surprises many parents: asthma doesn’t look the same in every child. Some children wheeze loudly. Others just cough — persistently, especially at night. Some only have symptoms when they run. Some seem fine most of the time and then suddenly can’t catch their breath during a cold. Asthma is not a single presentation. It’s a spectrum, and understanding where your child falls on that spectrum is the foundation of good care.
Asthma symptoms vs. common colds vs. allergies
One of the hardest parts of recognizing asthma in a child is that its symptoms overlap heavily with things that are much more common and much less concerning.
A cold gives your child a cough, a runny nose, maybe a low fever. It lasts a week or two and goes away. Allergies give your child a runny nose, itchy eyes, sneezing, and sometimes a cough — and they come and go with the seasons or with exposure to specific triggers. Both of these are normal parts of childhood.
Asthma looks different because of the pattern. The cough that sticks around long after the cold is over — two, three, four weeks later, your child is still coughing, especially at night or early in the morning. The wheeze that shows up every time they exercise hard, not just once but repeatedly. The breathing difficulty that seems disproportionate to the illness — a mild cold that turns into two weeks of labored breathing when other kids bounce back in days. Chest tightness that your child might describe as their chest feeling “tight” or “funny” or that they “can’t get enough air.”
The nighttime and early morning pattern is particularly telling. Asthma symptoms tend to be worse during these hours because of natural changes in airway function. If your child consistently coughs after they fall asleep or wakes up coughing in the early morning hours, that’s a signal worth paying attention to.
Allergies and asthma are also closely related — they aren’t just look-alikes. In many children, allergies are a primary trigger for asthma symptoms. Untreated allergic rhinitis (the stuffy, runny nose) can make asthma worse by increasing overall airway inflammation. So if your child has allergies and also has a persistent cough or breathing issues, the two may be connected rather than coincidental.
The key question Dr. Porter asks is not whether your child had one episode of wheezing. It’s whether there’s a pattern — recurring symptoms, triggered by identifiable things, following a recognizable timeline. One wheeze during a bad respiratory virus is common. A pattern of wheezing, coughing, or breathing difficulty that keeps coming back is a conversation worth having.
When to bring it up with your pediatrician
You don’t need to wait for a dramatic episode to bring up your concerns. In fact, most childhood asthma is identified not through emergencies but through parents noticing patterns over time and raising them with their pediatrician.
Here are the signals that it’s worth having the conversation. Your child’s cough lasts significantly longer than their colds — other kids recover in a week, yours is still coughing three weeks later. Your child coughs or wheezes during or after physical activity. Nighttime coughing is disrupting their sleep — or yours. Your child seems to get “bronchitis” or “chest colds” more often than their peers. They avoid running or physical play because it makes them feel bad. A family member — parent, sibling — has asthma or significant allergies.
For many families in Richardson, the conversation starts naturally during a routine physical exam where Dr. Porter is already listening to your child’s lungs and asking about respiratory patterns. These visits are built for exactly this kind of observation — catching things that might not prompt a standalone appointment but matter when they’re part of a bigger picture.
When you do bring it up, it helps to have some details ready. How long has the cough or breathing trouble been going on? When does it happen — nighttime, during exercise, after colds, during certain seasons? Does anything seem to make it better or worse? But even if you don’t have all of that organized, it’s okay. Dr. Porter will walk you through the questions that matter.
The Diagnostic Journey at Our Richardson Office
What the first visit looks like
When you bring your child to the N Floyd Rd office with breathing concerns, the visit starts with a thorough conversation — not a rush to tests or prescriptions.
Dr. Porter will ask about your child’s respiratory history in detail. How often are they coughing? Is it wet or dry? When does it happen — at night, during exercise, when they’re around certain environments? How long have the symptoms been present? Does anything consistently trigger them? How quickly do they recover from colds compared to other kids?
He’ll also ask about your family history, because asthma has a strong genetic component. If one or both parents have asthma, allergies, or eczema — a triad sometimes called the “atopic march” — that raises the probability significantly. He’ll ask about the home environment: pets, smoking exposure, mold issues, type of heating and cooling system. And he’ll ask about your child’s broader health — their growth, their activity level, their sleep quality — because asthma doesn’t exist in isolation.
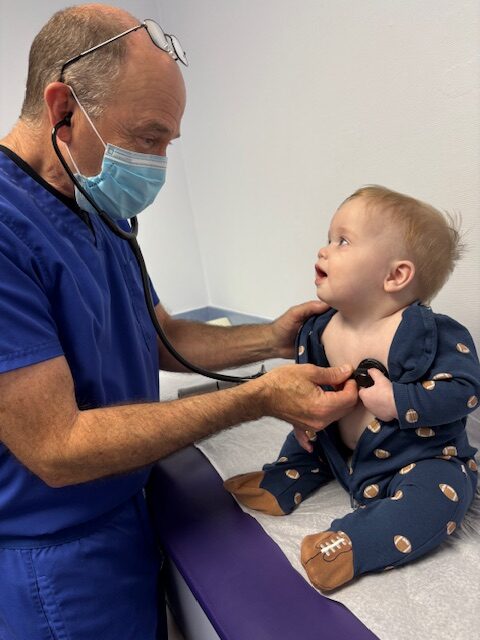
The physical exam is focused but thorough. Dr. Porter will listen to your child’s lungs carefully — not just for wheezing, which may or may not be present at the time of the visit, but for prolonged expiration, decreased air movement, or any sounds suggesting airway narrowing. He’ll look at the nose for signs of allergic inflammation. He’ll observe your child’s breathing pattern and effort.
One thing Dr. Porter will be transparent about from the start: asthma diagnosis in children, especially young children, isn’t always a straightforward one-visit process. There’s no single blood test or scan that confirms asthma the way a strep test confirms strep throat. Diagnosis is built on history, physical findings, response to treatment, and sometimes objective lung function testing. It takes thoroughness, and he’d rather be thorough than premature.
Diagnostic tools and approach
The tools Dr. Porter uses depend on your child’s age, the severity of symptoms, and how clear the clinical picture is.
Spirometry is the gold standard for measuring lung function. It’s a simple breathing test where your child blows into a device that measures how much air they can exhale and how fast they can do it. The key numbers are the FEV1 (how much air your child can forcefully exhale in one second) and the FEV1/FVC ratio (which compares that one-second burst to the total amount of air they can exhale). In asthma, these numbers are often reduced — and they improve after a dose of a bronchodilator (rescue inhaler), which is a hallmark finding. Spirometry is reliable in children who are roughly five years old and above and can follow the instructions to blow hard and long. For younger children, the test isn’t practical, and Dr. Porter relies on other approaches.
Peak flow monitoring is a simpler tool that measures how fast your child can blow air out. It’s less precise than spirometry but useful for ongoing monitoring at home. Dr. Porter may give your family a peak flow meter to track your child’s numbers over time, which helps identify trends, triggers, and early signs of worsening.
For younger children who can’t perform spirometry, or for cases where the symptoms are suggestive but not conclusive, Dr. Porter often uses a trial treatment approach. This means prescribing a short course of asthma medication — typically an inhaled corticosteroid or a bronchodilator — and observing whether symptoms improve. If a child’s chronic cough or recurrent wheezing resolves with asthma treatment and returns when it’s stopped, that response itself is strong diagnostic evidence.
Throughout this process, Dr. Porter is also thinking about what else the symptoms could be. Recurrent viral wheeze — wheezing that only happens during viral infections and resolves completely between episodes — is common in preschoolers and doesn’t always mean asthma. Vocal cord dysfunction can mimic asthma in older children and teens. Gastroesophageal reflux can cause a chronic cough that looks like asthma. Foreign body aspiration — a small object lodged in the airway — can cause persistent coughing or wheezing on one side. Part of the diagnostic process is systematically considering these alternatives so the right condition gets the right treatment.
How long the process takes
For some children, the picture is clear at the first or second visit — classic symptoms, family history, clear response to bronchodilator, abnormal spirometry. In those cases, Dr. Porter can make a confident diagnosis and start building a treatment plan promptly.
For others, particularly children under five, the process takes longer. Young children wheeze for many reasons, and predicting which of them will go on to have persistent asthma versus outgrowing their symptoms is one of the harder calls in pediatric medicine. Dr. Porter may monitor over several months, observe the pattern across seasons, and use trial treatments before committing to a formal asthma diagnosis. This isn’t indecision — it’s responsible medicine. Labeling a two-year-old with asthma prematurely can lead to unnecessary long-term medication. Failing to recognize asthma in a child who has it leads to preventable suffering. He navigates that balance carefully.
What he promises is that you’ll never be left in the dark. At every step, he’ll explain what he’s seeing, what he’s thinking, and what comes next.
Delivering the diagnosis and building the first plan
When Dr. Porter is confident in the diagnosis, the conversation with your family is direct, thorough, and practical.
He’ll explain what asthma means for your child specifically — not asthma in the abstract, but your child’s particular pattern, severity, and triggers. He’ll make sure you understand what’s happening in the airways, why certain things make it worse, and why the medications he’s recommending work the way they do. Parents who understand the “why” behind the treatment plan are far more effective at managing their child’s asthma than parents who are just handed prescriptions and told to follow up.
He’ll introduce the concept of the asthma action plan — a written document that becomes your family’s roadmap for daily management, symptom response, and emergencies. Building that plan together is what happens next.
What asthma doesn’t mean is that your child’s life needs to shrink. It doesn’t mean no sports, no outdoor play, no sleepovers, no summer camp. It means your child has a condition that requires management, and with the right management, they can do everything their peers do. Dr. Porter makes this point explicitly, because the fear of limitation is often the first thing parents feel when they hear the word “asthma.”
Understanding Your Child’s Asthma
Asthma severity classifications
Not all asthma is the same, and the treatment your child needs depends heavily on where their asthma falls on the severity spectrum. Dr. Porter uses the standard classification system to categorize your child’s asthma at diagnosis and reassesses it regularly, because severity can change over time.
Intermittent asthma is the mildest form. Symptoms occur two days a week or fewer. Nighttime awakenings happen two times a month or fewer. Your child uses a rescue inhaler two days a week or fewer. Between episodes, they’re completely symptom-free. Lung function is normal. Most children with intermittent asthma need only a rescue inhaler and don’t require daily medication.
Mild persistent asthma means symptoms more than twice a week but not every day. Nighttime awakenings three to four times a month. Rescue inhaler use more than two days a week. Symptoms are noticeable but don’t significantly limit daily activities. This is typically where daily controller medication enters the picture.
Moderate persistent asthma involves daily symptoms. Nighttime awakenings more than once a week. Rescue inhaler use daily. Symptoms limit some normal activities. Lung function is reduced. These children need daily controller medication and may need more than one type.
Severe persistent asthma means symptoms throughout the day. Frequent nighttime awakenings. Rescue inhaler use multiple times daily. Significant activity limitation. Lung function is significantly reduced. These children require aggressive daily treatment, often multiple medications, and closer monitoring.
These categories aren’t permanent labels. A child who starts with moderate persistent asthma may, with good treatment and trigger management, move to mild persistent. A child with mild persistent asthma who goes through a bad allergy season may temporarily look moderate. Dr. Porter reassesses at every follow-up visit and adjusts the plan accordingly.
The asthma action plan — your family’s roadmap
Every child with asthma in Dr. Porter’s practice gets an asthma action plan. This isn’t a suggestion — it’s a requirement of good care. The action plan is a single-page document that tells you, your child, and anyone else involved in your child’s care exactly what to do in every scenario.
The plan uses a green-yellow-red zone system that’s intuitive and easy to follow.
Green zone means your child is doing well. Breathing is good, no coughing or wheezing, sleeping through the night, able to play and exercise normally. In this zone, you continue the daily controller medication as prescribed and live life normally.
Yellow zone means symptoms are starting. Coughing, wheezing, chest tightness, waking at night, needing the rescue inhaler more than usual. The plan specifies exactly what to do: use the rescue inhaler, potentially increase the controller medication temporarily, monitor closely, and call the office if things don’t improve within a specified timeframe.
Red zone means this is serious. Severe breathing difficulty, rescue inhaler isn’t helping, your child can’t talk in full sentences, lips or fingernails are changing color. The plan tells you to give specific emergency medications, call 911 or get to the ER immediately, and call Dr. Porter’s office.
What makes this plan effective isn’t just having it — it’s how Dr. Porter builds it with you. He walks through each zone, explains the decision points, makes sure you can recognize the transitions, and answers every question. He tailors the specific medications and doses to your child. And he makes sure the plan goes where it needs to go: a copy at home, a copy in your child’s backpack, a copy with the school nurse, copies with any regular caregivers — grandparents, babysitters, the other parent’s household.
For families in the Richardson ISD, Plano ISD, and Garland ISD systems, Dr. Porter’s office is experienced in working with school nurses to ensure the action plan is on file and that your child has access to their rescue inhaler during the school day. He provides the medical documentation schools require and can communicate directly with the school nurse when needed.
Treatment — Dr. Porter’s Approach
The two categories of asthma medication
Understanding the difference between the two main types of asthma medication is one of the most important things you can learn as a parent of a child with asthma. Getting this distinction right affects how consistently you give the medication, how you respond to symptoms, and how well your child’s asthma is controlled.
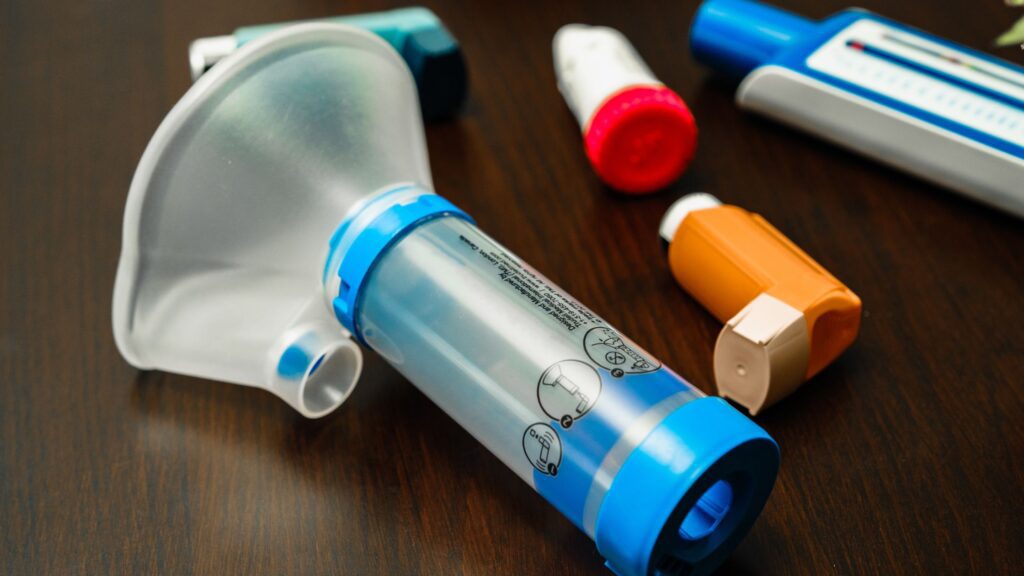
Controller medications are taken every day, usually once or twice daily, whether or not your child is having symptoms. Their job is to reduce the chronic inflammation inside the airways — to keep the swelling down, the mucus production low, and the airways calm and open. They don’t provide instant relief. They work gradually, over days and weeks, to prevent symptoms from happening in the first place. The most common controller medications are inhaled corticosteroids — medications like fluticasone (Flovent), budesonide (Pulmicort), and beclomethasone (QVAR). For children who need more control, combination inhalers that pair an inhaled corticosteroid with a long-acting bronchodilator may be used. Leukotriene modifiers like montelukast (Singulair) are another option, taken as a daily pill or chewable tablet.
Rescue inhalers — most commonly albuterol (ProAir, Ventolin) — are used only when symptoms occur. They work within minutes by relaxing the tightened muscles around the airways, opening them up and making it easier to breathe. They treat the immediate symptom but do nothing about the underlying inflammation. Think of it this way: the controller is the fire prevention system, and the rescue inhaler is the fire extinguisher. You need both, but if you’re using the fire extinguisher every day, the prevention system needs adjustment.
Dr. Porter teaches proper inhaler technique during office visits, not just at diagnosis but at follow-up visits as well, because studies consistently show that a large percentage of children (and adults) use their inhalers incorrectly, which reduces their effectiveness. For younger children, this means using a spacer with a metered-dose inhaler or using a nebulizer. For older children and teens, it may mean transitioning to a dry powder inhaler. He’ll make sure your child can demonstrate proper technique before leaving the office.
Starting treatment — matching the plan to the severity
Dr. Porter doesn’t prescribe the same regimen for every child. The starting treatment is matched to the severity classification, your child’s age, and the clinical picture.
A child with intermittent asthma may need nothing more than a rescue inhaler to use when symptoms appear. No daily medication, no complex routine — just albuterol on hand for the occasional episode.
A child with mild persistent asthma will typically start on a low-dose inhaled corticosteroid as a daily controller, plus a rescue inhaler for breakthrough symptoms. This is the most common starting point and is effective for a large number of children.
A child with moderate persistent asthma may start on a medium-dose inhaled corticosteroid, or a low-dose inhaled corticosteroid combined with a long-acting bronchodilator, depending on age and the specifics of their symptoms.
A child with severe persistent asthma will start on more aggressive treatment — higher-dose controllers, combination therapies, and potentially a referral to a pulmonologist or allergist for additional support.
In every case, Dr. Porter starts with the simplest regimen that’s likely to achieve good control. He’d rather start appropriately and step up if needed than overtreat from the beginning. And he explains his reasoning — why this medication, why this dose, what he expects to see, and when he’ll reassess.
Stepping treatment up or down
Asthma treatment is not static. It’s a dynamic process of adjustment based on how your child is actually doing — not how the textbook says they should be doing.
If your child’s symptoms aren’t well-controlled on the current plan — they’re still coughing at night, still needing the rescue inhaler several times a week, still having activity limitations — Dr. Porter steps treatment up. That might mean increasing the dose of the current controller, adding a second controller medication, or adding a leukotriene modifier. Before stepping up, he’ll also recheck inhaler technique (because a perfectly prescribed medication used incorrectly won’t work), reassess trigger exposure, and make sure the diagnosis is right. Sometimes what looks like uncontrolled asthma is actually uncontrolled allergies, poor medication adherence, or a different condition altogether.
If your child’s symptoms have been well-controlled for an extended period — typically three months or more of good control — Dr. Porter considers stepping treatment down. This means gradually reducing medication to find the lowest effective dose. Stepping down is just as important as stepping up, because the goal is to use the least amount of medication needed to keep your child’s asthma controlled. There’s no reason to keep a child on medium-dose controller therapy if low-dose would work just as well. And for some children, stepping down eventually means stepping off daily medication entirely, while keeping a rescue inhaler on hand.
These adjustments happen during regular follow-up visits as part of Dr. Porter’s approach to ongoing pediatric health care — not in response to crises, but as a proactive, data-driven calibration that keeps your child on the right amount of treatment at every stage.
Daily Life With Asthma in North Texas
Managing triggers at home
Asthma triggers are the things in your child’s environment that provoke airway inflammation and symptoms. Identifying and reducing your child’s specific triggers is a critical part of asthma management — and it’s an area where Dr. Porter gives practical, realistic advice rather than handing over a list of impossible demands.
Common indoor triggers include dust mites (which thrive in bedding, carpeting, and upholstered furniture), pet dander (from cats, dogs, and other furry animals), mold (especially in bathrooms, basements, and areas with poor ventilation), cockroach allergens, tobacco smoke and vaping aerosol, and strong scents from cleaning products, candles, or air fresheners.
Dr. Porter doesn’t tell families to rip out all their carpet, get rid of their pets, and sterilize their homes. He helps you prioritize the changes that will make the biggest difference for your specific child. If dust mites are a trigger, encasing mattresses and pillows in allergen-proof covers is high-yield and affordable. Washing bedding weekly in hot water helps. Keeping humidity below 50% reduces dust mite populations. If pet dander is an issue, keeping the pet out of the child’s bedroom and using HEPA filtration can make a meaningful difference without rehoming the family dog.
Living in the Richardson and North Dallas area brings some specific environmental considerations. The humidity levels in North Texas — particularly during spring and summer — can promote mold growth indoors. The region’s HVAC systems run heavily, and dirty filters circulate allergens continuously. Dr. Porter recommends changing HVAC filters regularly (every one to three months), using high-quality pleated filters, and considering a HEPA air purifier in your child’s bedroom if environmental allergies are a significant trigger.
And while it shouldn’t need to be said, it does: if anyone in the household smokes, the single most impactful thing they can do for a child with asthma is to stop. Secondhand smoke is one of the most potent asthma triggers in children, and no amount of medication can fully compensate for ongoing smoke exposure.
Managing triggers at school and outdoors
Your child’s asthma doesn’t stop at the school door, and making sure the school is prepared to manage it is essential.
The foundation is getting the asthma action plan into the school’s hands. Dr. Porter’s office provides the documentation, and the plan should be on file with the school nurse and shared with every teacher, PE teacher, and coach who works with your child. Most critically, your child needs access to their rescue inhaler during the school day. In Texas, students are legally allowed to carry and self-administer prescribed asthma medication at school with proper documentation, and Dr. Porter’s office provides the necessary forms.
For families in Richardson ISD, Plano ISD, and Garland ISD, the practice is familiar with each district’s medication policies and can guide you through the paperwork. If your child’s school doesn’t have a full-time nurse, Dr. Porter can help you work with the campus health aide to ensure the plan is understood and accessible.
Outdoor triggers in North Texas follow a predictable calendar, and knowing it helps. Cedar pollen hits hard in December through February — the infamous “cedar fever” season. Grass pollen surges in late spring. Ragweed dominates the fall. Ozone levels climb during hot summer days, particularly in the Dallas–Fort Worth metro area, and high-ozone days can trigger asthma symptoms even in children whose asthma is normally well-controlled. And in recent years, wildfire smoke from distant fires has periodically degraded air quality across the region.
Dr. Porter recommends checking air quality before planning outdoor activities on high-risk days. AirNow.gov provides real-time air quality index data for the Richardson and Dallas area. On days when the AQI exceeds 100 (unhealthy for sensitive groups), your child may need to limit prolonged outdoor exertion or pre-treat with their rescue inhaler before going outside.
Asthma and sports/physical activity
This is where many parents’ anxiety spikes — and where Dr. Porter is most emphatic. Asthma should not stop your child from playing sports or being physically active. Period.
Exercise-induced bronchoconstriction — airway narrowing triggered by physical exertion — is common in children with asthma. It typically shows up as coughing, wheezing, chest tightness, or shortness of breath during or after vigorous activity. It can look like the child is just “out of shape,” but the pattern is specific: symptoms that come on during sustained exercise and resolve with rest.
The solution is not avoiding exercise. It’s managing it. The first-line approach is pre-treatment: having your child use their rescue inhaler (usually two puffs of albuterol) about 15 to 20 minutes before exercise. This opens the airways preemptively and prevents the bronchoconstriction from happening. A proper warm-up — five to ten minutes of gradually increasing activity before going full intensity — also helps.
Some sports are more asthma-friendly than others. Swimming, for example, is often well-tolerated because the warm, humid air above the pool is less likely to trigger symptoms than cold, dry air. But Dr. Porter won’t steer your child away from any sport they love. If your child wants to run cross-country or play basketball or join the soccer team, the management plan adapts to support that — not the other way around.
Coaches and PE teachers should know about your child’s asthma. They need to understand that your child may need to use an inhaler before practice, that symptoms during exercise are not a sign of being unfit, and that pushing through an asthma flare during physical activity is not safe. The asthma action plan should be in their hands, and your child should have their rescue inhaler accessible — in their sports bag, not locked in the nurse’s office across campus.
Sports readiness is something Dr. Porter assesses during a routine physical exam or anadolescent physical exam — he reviews asthma control as part of every sports clearance, ensuring your child is safe to participate and that the management plan is optimized for physical activity.
Seasonal flare-ups and how the practice prepares families
If you’ve lived in Richardson or the North Dallas area long enough, you know the seasons bring more than just weather changes. For children with asthma, each season carries specific risks, and Dr. Porter manages proactively rather than reactively.
Fall and winter are typically the highest-risk period for childhood asthma flare-ups — and not because of cold air, though that doesn’t help. The primary culprit is viral respiratory infections. RSV, influenza, common cold viruses — these infections hit hardest in the fall and winter months, and for children with asthma, a virus that gives another kid a runny nose can trigger a weeks-long asthma exacerbation. Dr. Porter often recommends stepping up controller therapy during the fall months preemptively, increasing the dose temporarily to build a buffer before viral season peaks. He’s also a strong advocate for flu vaccination in children with asthma, because influenza is one of the most predictable and preventable asthma triggers.
Spring brings the pollen surge — grass pollen in particular blankets the North Texas region from late March through May. For children whose asthma has an allergic component, this season can mean a significant uptick in symptoms. Dr. Porter may add or adjust allergy treatment during these months to keep the overall inflammatory load down.
Summer in North Texas means heat, ozone, and intense outdoor activity. High-ozone days are a real concern in the Dallas metro area, and children with asthma are among the most vulnerable populations. Dr. Porter talks with families at spring visits about monitoring air quality and adjusting outdoor activity plans during ozone alerts.
The theme across all seasons is the same: don’t wait for the flare-up and then react. Anticipate it, prepare for it, and adjust the plan ahead of time. That’s the approach Dr. Porter takes, and it’s one of the reasons his asthma patients tend to stay out of the emergency room.
When Asthma Overlaps With Allergies
The asthma-allergy connection
The relationship between asthma and allergies is not a coincidence — it’s biological. The majority of childhood asthma is allergic asthma, meaning that allergic inflammation in the airways is a primary driver of the disease. The same immune system overreaction that causes your child’s nose to run around cats or during pollen season is causing inflammation inside their lungs.
This means that in many children, you can’t fully control asthma without addressing the allergies that are fueling it. A child who’s on the right asthma controller medication but still sleeping with a dust-mite-loaded pillow and a cat on the bed may not achieve full control no matter how perfectly they use their inhaler. Treating the allergic component — through environmental changes, allergy medication, or immunotherapy — can be the missing piece that brings asthma under control.
Signs that your child’s asthma may have a significant allergic component include: symptoms that worsen during specific pollen seasons, clear triggers related to animal exposure or dusty environments, a personal history of eczema or food allergies (especially in early childhood), and a strong family history of allergic conditions.
When Dr. Porter refers to an allergist
Dr. Porter manages the allergic component of asthma for many of his patients directly — recommending environmental changes, prescribing antihistamines and nasal corticosteroids, and monitoring the interplay between allergy symptoms and asthma control.
But there are situations where an allergist adds significant value. If your child’s asthma is difficult to control despite appropriate treatment and good medication adherence, allergist evaluation can identify specific triggers through skin prick testing or specific IgE blood tests. Knowing exactly what your child is allergic to — not just a general suspicion, but specific allergens with measured sensitivity levels — allows for targeted avoidance strategies and opens the door to allergen immunotherapy (allergy shots or sublingual tablets), which can reduce allergic sensitivity over time and improve asthma control at its root.
Dr. Porter works with allergists in Richardson, Plano, and the greater North Dallas area, and when he refers, it’s a collaborative relationship rather than a handoff. The allergist handles the allergy-specific evaluation and treatment. Dr. Porter continues to manage the asthma itself, coordinates the overall plan, and ensures that the two sides of your child’s care are aligned. Shared action plans, consistent medication strategies, and open communication between providers are how this works in practice.
Emergency Situations
Recognizing an asthma emergency
Most asthma episodes respond to the rescue inhaler and the yellow-zone steps in your child’s action plan. But some don’t — and knowing the difference between a manageable flare and a true emergency can be lifesaving.
Red-zone symptoms that require immediate action include severe difficulty breathing where your child is visibly working hard to get air — you can see the muscles between their ribs pulling in with each breath, their nostrils are flaring, and their shoulders are moving up and down. The rescue inhaler has been given and isn’t providing relief, or relief lasts less than fifteen minutes before symptoms return. Your child can’t speak in full sentences because they can’t get enough air. Their lips, fingernails, or the skin around their mouth is turning blue or gray. They seem confused, drowsy, or panicked in a way that’s different from their usual distress.
If you see any of these signs, the protocol is clear. Give the rescue inhaler immediately — even if you’ve already given it recently — and call 911. Do not drive to the ER yourself if your child is in severe distress. Paramedics can administer treatments en route that you cannot.
When to use the ER vs. call the office
Not every concerning episode is a 911 situation. Dr. Porter helps families understand the distinctions.
True emergencies — ER or 911 immediately: the red-zone symptoms described above. Blue or gray discoloration. Rescue inhaler not working. Severe distress. Do not call the office first. Go.
Urgent but not emergency — call the office: your child is in the yellow zone and not improving with the steps in the action plan. They’re coughing and wheezing but not in severe distress. They needed the rescue inhaler more than every four hours. They’re having a worse-than-usual episode but are still able to talk, eat, and function. Call Dr. Porter’s office at (972) 235-6911 during business hours for same-day guidance, or use the after-hours nurse advice line in the evenings and weekends. The nurses can help you determine whether your child needs to be seen urgently, can manage at home with adjustments, or should go to an ER.
After an ER visit: if your child does end up in the emergency room for an asthma exacerbation, Dr. Porter wants to see them in the office within a few days of discharge. ER visits are a signal that the current management plan needs reassessment. He’ll review what happened, evaluate whether the severity classification needs to change, adjust medications, and update the action plan. An ER visit for asthma should never just be a one-time event that gets forgotten — it’s data that informs better ongoing care.
Ongoing Care and Monitoring
How the practice monitors asthma over time
Asthma is a chronic condition, and chronic conditions require ongoing attention. Dr. Porter doesn’t diagnose asthma, hand you a prescription, and send you off. He monitors your child’s asthma at regular intervals, adjusting the plan as needed based on real-world data.
How often you come in depends on where your child’s asthma is. Newly diagnosed children, or those whose asthma is not yet well-controlled, are typically seen every one to three months. Once asthma is stable and well-controlled, visits spread out to every three to six months. But they don’t stop.
At each visit, Dr. Porter systematically assesses control. How often has your child had symptoms since the last visit? How many nights have they been woken up by coughing or wheezing? How often have they needed the rescue inhaler? Have they missed any school or avoided any activities because of asthma? Has the peak flow been stable or trending down? He’ll re-listen to the lungs, review and possibly repeat spirometry, and check inhaler technique.
Based on that information, he’ll decide whether to maintain the current plan, step up, or step down. He’ll also reassess the severity classification — because a child who was moderate persistent a year ago may be mild persistent now, or vice versa.
These visits are woven into your child’s broader care schedule alongside routine physical exams and well-child visits, so asthma management doesn’t feel like a separate burden — it’s integrated into the ongoing relationship between your family and Dr. Porter’s practice.
Adjusting care as your child grows
Asthma management isn’t the same at age three as it is at age eight as it is at age fifteen. Dr. Porter adjusts the approach as your child develops — not just the medications, but the way care is delivered and who’s responsible for managing it.
For toddlers and preschoolers, asthma management is entirely parent-driven. Medications are typically delivered via nebulizer because young children can’t effectively use an inhaler. The action plan lives in the parent’s hands, and every dose, every observation, and every decision is yours.
For elementary school-age children, there’s a gradual transition. Many children move from nebulizers to metered-dose inhalers with spacers, which are portable and much faster. Children begin learning what their symptoms feel like and can start to recognize when they’re moving into the yellow zone. The action plan starts to include the child — not as the decision-maker, but as a participant who understands what’s happening in their body.
For adolescents, the shift toward self-management accelerates. Teens can use dry powder inhalers independently. They should know their medication names and doses, understand their triggers, be able to use their rescue inhaler correctly without supervision, and be able to articulate their needs to coaches, teachers, and eventually their own future providers. Dr. Porter talks directly to teens during visits — not over their heads to the parent — and involves them in treatment decisions. This is preparation for adulthood, where they’ll need to manage their asthma on their own.
Preparing for independence also means preparing for situations: sleepovers, school trips, summer camp, sports travel, and eventually leaving for college. Dr. Porter works with families to make sure the practical logistics are in place — that your child has medication with them, that responsible adults in those settings have the action plan, and that your child has the confidence to advocate for themselves when you’re not there.
The Long-Term Outlook
What research says about childhood asthma across the lifespan
The long-term picture for childhood asthma is more encouraging than most parents expect at the time of diagnosis. With proper management, the vast majority of children with asthma lead completely normal, fully active lives. They go to school, play sports, have sleepovers, go to camp, and eventually go to college and build careers — all with asthma as a manageable background condition rather than a defining limitation.
The research shows that early, consistent treatment matters. Children whose asthma is identified and managed early tend to have better lung function long-term, fewer hospitalizations, less airway remodeling (permanent structural changes from chronic inflammation), and better quality of life than children whose asthma goes unrecognized or undertreated for years.
That’s the case for not waiting. If your child has symptoms that suggest asthma, getting the evaluation done now — not next year, not when it gets worse — is an investment in their long-term respiratory health.
Can kids outgrow asthma? — the honest, nuanced answer
Roughly half of children diagnosed with asthma in early childhood will see their symptoms improve significantly or resolve entirely by adolescence. Children with mild intermittent asthma, children without a strong allergic component, and children who don’t have a family history of asthma are more likely to outgrow it.
But “outgrowing” asthma doesn’t always mean it’s gone permanently. Some people whose childhood asthma appeared to resolve see symptoms return later in life — during pregnancy, after a major respiratory infection, or when exposed to new environmental triggers. The airway sensitivity may persist even when symptoms don’t.
Dr. Porter doesn’t promise that your child will outgrow asthma, and he doesn’t manage asthma as though they definitely won’t. He manages the condition as it presents today, watches for improvement, steps treatment down whenever it’s safe to do so, and keeps a long-term perspective. If your child does outgrow their symptoms, that’s wonderful — and you’ll have the tools and knowledge to recognize it if symptoms ever return.
How Dr. Porter helps families plan for transitions
Just like with other chronic conditions he manages, Dr. Porter pays close attention to the transition points in your child’s life when asthma management needs to adapt.
The move from elementary to middle school means your child is changing classrooms throughout the day, potentially has no relationship with a school nurse, and is increasingly responsible for their own medication. Dr. Porter makes sure the action plan is updated for the new school, that your child knows how to carry and use their inhaler independently, and that at least one adult at the school knows your child has asthma.
The move to high school brings organized sports with intense practice schedules, increased independence, peer pressure to downplay medical needs, and the beginnings of the drive toward self-management. Dr. Porter talks directly with teens about the importance of not skipping their controller medication, carrying their rescue inhaler, and communicating with coaches.
Leaving for college is the transition that demands the most preparation. Your child needs to know their full medication list, understand their triggers, be able to refill prescriptions, know when to seek medical care, and have a relationship (or be ready to build one) with a new provider. Dr. Porter helps families prepare for this well before move-in day — transferring records, writing a comprehensive summary for a new provider, and making sure the young adult has the knowledge and confidence to manage independently.
Building self-management skills over time
The goal of pediatric asthma care is not to manage a child perfectly until they turn eighteen and then hope for the best. It’s to build, gradually and deliberately, a young person who understands their condition and can manage it themselves.
This starts small. A six-year-old learns to tell their parent when their chest feels tight. An eight-year-old learns to use their inhaler with a spacer independently. A ten-year-old learns to recognize their triggers and make basic decisions — like going inside when the air quality is bad. A fourteen-year-old can explain their asthma to a new coach, administer their own pre-exercise treatment, and follow their action plan without prompting.
Dr. Porter builds these skills incrementally through years of care. He involves children in their own visits at age-appropriate levels, explains medications to them directly, and treats them as partners in their own health. By the time they leave his practice, they’re not dependent on a parent’s memory or a pediatrician’s instructions. They own their asthma management — and that ownership is the most important thing he can give them.
Why ongoing care matters even when symptoms are well-controlled
There’s a natural temptation, once asthma is stable, to stop the controller medication or stop coming to follow-up visits. If it’s not broken, why maintain it?
The answer is that asthma control feels like the absence of disease, but it’s actually the presence of effective treatment. The controller medication is keeping the airways calm. The trigger avoidance strategies are preventing flare-ups. The regular monitoring is catching subtle changes before they become problems. Remove any of those elements, and the stability can unravel — sometimes gradually, sometimes suddenly.
Dr. Porter encourages families to maintain the rhythm of care even during the good stretches. A brief check-in every few months, a spirometry test, a review of the action plan, a conversation about any changes at home or school — these small investments prevent the big setbacks. And they keep the door open for stepping down medication when the time is right, done carefully and under observation rather than unilaterally at home.
If you’ve read this far, you now understand more about your child’s asthma — or potential asthma — than most parents ever do. That understanding is your greatest tool. It’s what allows you to recognize symptoms early, follow a treatment plan consistently, advocate for your child at school, respond calmly in an emergency, and help your child build the skills they’ll need to manage their own health for a lifetime.
Dr. Porter’s approach to childhood asthma has always been the same: know the child, partner with the family, build a plan that actually fits your life, and adjust it as things change. Whether your child is wheezing for the first time or has been managing asthma for years, the commitment is the same — careful attention, clear communication, and a genuine investment in your child’s ability to live fully and breathe easily.
If you’re ready to schedule an asthma evaluation, have questions about your child’s current treatment, or want a second opinion on an existing diagnosis, we’re here.
John R. Porter, MD, PA 1112 N Floyd Rd #10 Richardson, TX 75080 (972) 235-6911
Common Questions From Richardson-Area Parents
Are inhaled steroids safe for my child long-term?
This is the most common concern Dr. Porter hears, and he addresses it directly. Inhaled corticosteroids are not the same as the anabolic steroids you hear about in sports scandals, and they’re not the same as oral steroids (like prednisone) that carry significant side effects with long-term use. Inhaled corticosteroids are delivered in very small doses directly to the airways, where they work locally. Only a tiny fraction enters the bloodstream.
Decades of research have confirmed that inhaled corticosteroids are safe for long-term use in children when used at appropriate doses. There can be a small effect on growth velocity in the first year or two of use — roughly half a centimeter — but this doesn’t affect final adult height. The risk of uncontrolled asthma — emergency room visits, hospitalizations, missed school, impaired lung development, and the cascading effects on your child’s quality of life — far outweighs the minimal risk of properly dosed inhaled steroids.
That said, Dr. Porter doesn’t keep your child on more medication than they need. He regularly reassesses and steps down when asthma is well-controlled, always looking for the lowest effective dose.
Will my child become dependent on their inhaler?
Asthma medication is not addictive. Your child won’t become “dependent” on their inhaler in the way people become dependent on habit-forming substances. What can happen is that stopping controller medication causes symptoms to return — but that’s not dependence, that’s the underlying disease reasserting itself because the treatment was removed.
If your child’s asthma is well-controlled for a sustained period, Dr. Porter will attempt to step down and potentially discontinue daily medication. Some children achieve that. Others need daily controller therapy long-term because their asthma requires it. In either case, the medication is treating a real condition — not creating a dependency.
Can my child outgrow asthma?
Many parents hope for this, and the answer is nuanced. Some children — particularly those with mild asthma that started in early childhood — do see their symptoms decrease significantly or disappear entirely by adolescence or early adulthood. The airways mature, the immune system changes, and the triggers that once caused problems no longer have the same effect.
But “outgrowing” asthma is not guaranteed, and it’s not something to plan around. Many children carry their asthma into adulthood. Some children whose symptoms disappear in their teens see them return in their twenties or thirties. The underlying airway sensitivity may remain even when symptoms are absent. Dr. Porter’s approach is to manage the asthma your child has today, monitor for improvement, and celebrate it when it comes — without making promises about a specific outcome.
Is it asthma or just a cough?
A cough is a symptom. Asthma is one of many possible causes. The way to tell the difference is the pattern: does the cough recur? Does it follow specific triggers — exercise, cold air, viral infections, allergen exposure? Is it worse at night? Does it respond to bronchodilator medication? A one-time cough after a cold is probably just a cough. A cough that keeps coming back, follows identifiable patterns, and responds to asthma treatment is probably asthma. Dr. Porter sorts this out through careful history, observation, and sometimes trial treatment.
Can my child play sports with asthma?
Absolutely. This question gets a one-word answer first, and then the explanation. Exercise-induced symptoms are manageable with pre-treatment, proper warm-ups, and good baseline asthma control. Olympic athletes have won gold medals with asthma. Your child can play soccer, run track, swim competitively, or do anything they love. The management plan adapts to support the activity — the activity doesn’t shrink to accommodate the asthma.
What’s the difference between a nebulizer and an inhaler?
Both deliver the same medication — the difference is the delivery method. A nebulizer turns liquid medication into a fine mist that your child breathes in through a mask or mouthpiece over about five to ten minutes. It’s commonly used for young children who can’t coordinate the technique required for an inhaler. A metered-dose inhaler (MDI) delivers medication in a pressurized puff — when used with a spacer (a tube that holds the medication in a chamber while your child breathes it in), it’s just as effective as a nebulizer and much faster. Dry powder inhalers are breath-activated and work well for older children and teens. Dr. Porter transitions your child to the most appropriate device for their age and ability.
Do you accept my insurance for asthma care?
Insurance coverage and accepted plans can change, so the best thing to do is call our Richardson office directly at (972) 235-6911. Our front desk team can verify your coverage and let you know about any out-of-pocket costs before your first appointment.
