How Do Pediatricians in Richardson, TX Support Mental Health?
If you are a parent in Richardson, it is hard to ignore how stress is showing up in kids today. School pressure, screen time, and sleep problems can pile up fast. That is why many families ask: How do pediatricians in Richardson, TX support mental health? A pediatrician often becomes the first safe place for children to talk about mood, behavior, focus, and anxiety. These concerns can show up as stomachaches, headaches, school refusal, or anger at home in children of all ages.
The American Academy of Pediatrics recommends mental and emotional health checks as part of regular well visits, using age-appropriate screening tools. That helps catch concerns early, before they grow into bigger problems. In simple terms, a pediatrician is often the front line for pediatric mental health in the community. They screen children, guide families, and connect them with local specialists when needed — and the range of pediatric services offered in Richardson, TX reflects just how broad that support can be.
If you have not talked about mental health at a well visit yet, the next visit is a good time to start. It also helps to know the qualifications your pediatrician in Richardson, TX holds so you feel confident in the care your child receives.
Next step: Bring up mental health screening at your child’s next well visit and ask what tools the office uses.
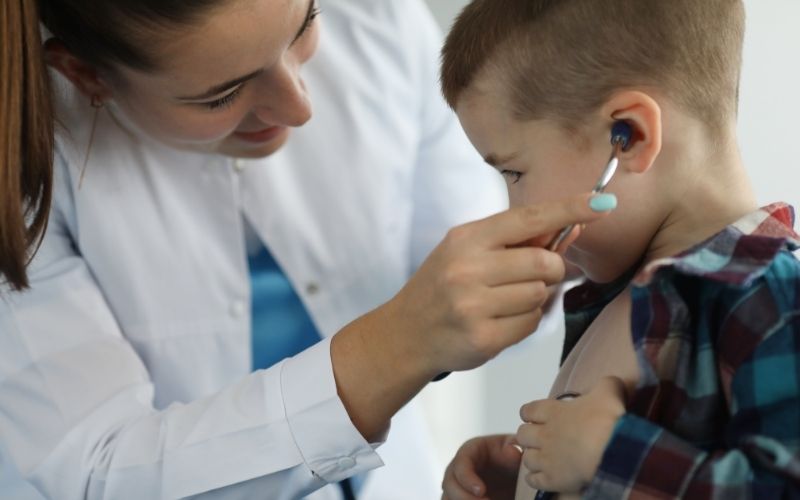
Standardized Screening Protocols
Mental health support often starts with a simple step: asking the right questions at the right ages. Pediatricians use short, standardized tools to spot concerns early. These tools do not replace a full diagnosis. They help decide what needs a closer look.
In Richardson, many families notice that school demands feel heavier in middle school and high school. That is when anxiety, sadness, and attention issues can become more obvious. A good screening process helps the pediatrician separate normal stress from a problem that needs support.
Here is a clear tool-by-age overview that many pediatric offices follow:
| Age Group | Screening Tool | Frequency | Identifies |
| 9 to 18 months | ASQ: SE (social-emotional) | Well visits | Social-emotional delays, attachment concerns |
| 18 to 60 months | SWYC (emotional/behavioral) | Regular visits | Early behavior concerns, developmental flags |
| 4 to 12 years | PSC-17 (Pediatric Symptom Checklist) | Annual, or as needed | Attention issues, anxiety signs, behavior concerns |
| 12 to 18 years | PHQ-9 (depression) and GAD-7 (anxiety) | Annual, and as needed | Depression symptoms, generalized anxiety signs |
What this looks like in real life:
- You fill out a short form in the office or on a patient portal.
- The pediatrician reviews the results with you and your child.
- You talk about what is happening at school and at home.
- You decide on a plan, which might include follow-up visits, school coordination, therapy, or referral.
If you want to learn what to expect from routine visits, review the practice approach on the Routine Physical Exam page.
Vanderbilt ADHD Assessment and Medical Review
For ADHD, pediatricians often use the Vanderbilt assessment. It includes short parent and teacher forms. This helps the doctor compare what is happening at home and at school. The forms look at attention, hyperactivity, and how symptoms affect grades, behavior, and relationships.
In Richardson, coordination can include school nurse input or a counselor check-in, especially when parents are trying to decide if a child needs classroom supports. When the pediatrician has clear school feedback, the next steps become more focused and less stressful.
In-Office Brief Interventions
Many parents think mental health care always means a referral. Sometimes it does. But pediatricians can often start support right in the office, especially when concerns are mild to moderate.
These visits are usually short and practical. The goal is to reduce symptoms and improve day-to-day function while the family builds a longer plan.
Common in-office supports include:
- Parent Management Training Basics
- Simple positive reinforcement schedules
- Clear rules, short directions, and consistent follow-through
- Small rewards that match the child’s age
- Anxiety Coping Skills
- Slow breathing practice
- A simple “fear ladder” for gradual practice steps
- Planning for tough moments like test days or social events
- Sleep Hygiene Protocols
- Screen-free time before bed
- Consistent bedtime and wake time
- Simple bedtime routine, same order each night
- ADHD Behavior Plans
- Daily report cards from teachers
- Token systems at home
- Clear homework routine with short breaks
- Suicide Risk Check and Safety Planning
- Direct questions about safety when warning signs appear
- A clear plan for who to call and what to do next
- Immediate referral or emergency care when needed
If your child has physical symptoms linked to stress, your pediatrician can also check for common medical causes. That helps you avoid guessing.
For general pediatric support and children health topics the office treats, see Child Healthcare.
Medication Management Capabilities
When symptoms disrupt school, sleep, or daily life, medication may be part of the plan. Pediatricians can prescribe and manage many first-line medications, especially for ADHD and some anxiety or depression cases. They also monitor side effects and track improvement.
Medication should never feel like a “quick fix.” A responsible plan includes:
- a clear reason for treatment
- a baseline symptom check
- follow-up visits at set times
- side effect education
- coordination with therapy or school supports when needed
Here is a simplified table of common first-line options and monitoring steps:
| Condition | First-Line Medication | Monitoring Schedule | Notes |
| ADHD | Methylphenidate options | Monthly at first, then every 3 months | Check appetite, sleep, growth, and school feedback |
| Anxiety | SSRI options like sertraline | Monthly early on | Watch mood changes, sleep, and stomach symptoms |
| Depression | SSRI options like fluoxetine | Weekly check-ins early, then monthly | Safety planning and close follow-up are key |
Important: Some cases require specialized care from a child psychiatrist, especially if symptoms are severe, safety is a concern, or there are complex diagnoses. A pediatrician helps decide when specialist care is needed.
Richardson Mental Health Referral Network
A strong pediatric office does not try to handle everything alone. Pediatric providers build a referral network so families can get help without starting from zero.

Below is a practical example of how referral pathways often look for Richardson-area families. Exact availability changes, so the pediatric office helps you confirm options that match insurance and timing.
| Pediatric Practice | Primary Psychiatrist Referral | Therapy Partners | Typical Wait Time |
| John R. Porter, MD, PA | ADHD-focused psychiatry options | Local CBT therapists | Often, a few weeks |
| Renner Pediatrics | Behavioral health partner options | Play therapy providers | Several weeks |
| Richardson pediatric groups | Children’s behavioral networks | Teen-focused therapy options | Several weeks |
| Large health systems | Internal behavioral programs | Network psychologists | Sometimes faster |
Crisis resources matter too. If a child is in danger, has a suicide plan, or you cannot keep them safe at home, go to the nearest emergency room right away. For urgent crisis support, many families use 988 for immediate guidance.
If you need to set up a visit to talk through concerns and next steps, you can book a pediatric appointment with the office.
Preventive Mental Health Strategies
Prevention sounds simple, but it works best when it is specific. Here is a parent-friendly checklist that pediatricians often recommend to build resilience and reduce stress.
Preventive Checklist
- Keep screen time limits realistic, aim for under 2 hours of non-school screen time most days.
- Make sleep consistent, same bedtime and wake time on school nights
- Eat together as a family when possible, even if it is shorter meals on busy days
- Balance activities, avoid stacking too many late practices and tutoring sessions
- Protect downtime, kids need unplanned time too
- Model healthy coping, kids watch how adults handle stress
- Keep communication open, ask one direct question daily: “What was hard today?”
Small changes done consistently are easier than big changes done once.
School and Community Coordination
Mental health support often runs through school. Pediatricians can help parents prepare for school meetings and paperwork. This may include:
- guidance for 504 plans and IEP conversations
- documentation for classroom supports
- coordination with counselors when parents sign releases
- behavior plan collaboration when attention or anxiety affects grades
In Richardson, many families also use school counseling resources, support services, and community programs when available. A pediatrician provides care guidance to help you decide which resource matches the child’s needs and which issues need a higher level of care.
Frequently Asked Questions
When should I talk to a pediatrician about my child’s anxiety in Richardson, TX?
Talk at the first sign it affects sleep, school, friends, or daily routines. Early support is easier.
What screening tools do pediatricians use for teen depression?
Many use PHQ-9-style tools for teens. They also ask direct safety questions when needed.
Can a pediatrician help with ADHD treatment near Plano?
Yes, many pediatricians manage ADHD with school forms, Vanderbilt assessments, and follow-ups.
What if my child refuses school because of stress?
A pediatrician can screen for anxiety, sleep problems, and depression, then guide the next steps.
Do pediatricians prescribe medication for anxiety or depression?
Some do for mild to moderate cases with close monitoring. They refer to psychiatry when needed.
How do I get a child psychiatrist referral near Spectrum Blvd?
Ask your pediatrician for local referral options and help matching insurance and wait times.
What should I bring to a mental health visit?
Bring school feedback, teacher notes if available, a symptom timeline, and any past evaluations.
Start the Conversation Today
If you are not sure how to bring this up, use this simple script at your next well visit:
- “I want to talk about my child’s mood, stress, and behavior.”
- “Here is what we are seeing at home and at school.”
- “Can we do mental health screening today?”
- “If the screening shows concerns, what is the next step in Richardson?”
If you want a pediatrician who takes mental health seriously and keeps the plan clear, schedule a visit with John R. Porter, MD, PA, through the contact page. You will leave with a practical next step, whether that is monitoring, in-office support, or a referral path.
