What are Common Pediatric Illnesses?
Your child wakes up coughing at 3 a.m. You check their forehead, you listen for wheezing, and you wonder, is this a cold, croup, or something more serious? These moments are why parents search for common pediatric illnesses. Most childhood illnesses are mild, but it helps to know what you are looking at and what to do next.
Most young kids catch a lot of viruses. In fact, many children average 8–10 respiratory infections each year before age 2. That can feel nonstop. The good news is that many common pediatric illnesses follow a predictable pattern. When you know the usual symptoms and the warning signs, you can often avoid panic and make a clear plan. Having a pediatrician who offers the right pediatric care services in Richardson, TX means those patterns get caught early, at a regular visit rather than an urgent one.

In this guide, we break down the top pediatric illnesses by age and how often they show up, what symptoms to expect, and when to get help in Richardson. We will cover respiratory infections, stomach bugs, rashes, vaccine-preventable illnesses, and rising chronic problems like asthma. Quick recognition and early steps at home can prevent many problems from getting worse and can reduce needless ER trips. It also helps to know the qualifications your pediatrician in Richardson, TX holds so you feel confident that the person guiding your child’s care has the training to back it up.
Respiratory Infections (60% of Visits)
Respiratory infections are the most common reason kids come to the doctor. Many are viral, and antibiotics do not help viral illnesses. A typical viral pattern looks like this:
- Days 1–3: sore throat, runny nose, low fever, mild cough
- Days 4–7: more cough and congestion, mucus may turn yellow or green
- Days 7–10: symptoms slowly improve, cough may linger
Parents often worry when mucus changes color. That change does not always mean a bacterial infection. Many common pediatric illnesses in the lungs and throat can look rough and still be viral.
Below is a simple season and red-flag guide you can use.
| Illness | Peak Season | Duration | Red Flags | Treatment |
| Common Cold | Year-round | 7–10 days | Fever > 3 days | Fluids, humidifier |
| Croup | Fall/Winter | 3–5 days | Stridor at rest | Steroids, ER if severe |
| Bronchiolitis (RSV) | Winter | 7–14 days | Rapid breathing | Oxygen if needed |
| Influenza | Winter | 5–7 days | High fever + aches | Antiviral if < 48 hrs |
| Pneumonia | Winter/Spring | 7–10 days | Chest pain, high fever | X-ray, antibiotics when bacterial |
Local note for Richardson: Back-to-school viruses often spike in late August and September. Many families also plan flu shots early in the fall. When more kids get vaccinated on time, fewer families deal with the flu at home.
Antibiotic myth to avoid:
Antibiotics do not treat colds, most coughs, most sore throats, or most cases of bronchitis. When antibiotics are not needed, they can cause side effects and raise resistance.
At-home help that actually works
- Saline spray or drops for stuffy noses
- Cool-mist humidifier at night
- Honey for cough in kids over age 1
- Rest and fluids
- Fever medicine only when your child is uncomfortable
Ear Pain and Ear Infections (80% kids by age 3)
Ear infections are one of the most common pediatric illnesses in toddlers. The main type is otitis media, which often follows a cold. Some kids do better with a “watch-and-wait” plan, especially if pain is mild and the child is older.
A common plan is:
- Pain control first (acetaminophen or ibuprofen if age-appropriate)
- Recheck if symptoms do not improve
- Antibiotics if the exam suggests bacterial infection, or if symptoms are severe
If your child has ear pain plus a high fever, severe fussiness, or drainage from the ear, it is time to call your pediatric office.
Gastrointestinal Illnesses (15% ER Visits)
Vomiting and diarrhea can lead to dehydration fast, especially in babies and toddlers. Many stomach bugs are viral. The biggest risk is not the virus itself; it is fluid loss.
How to judge dehydration at home
- Fewer wet diapers or fewer trips to the bathroom
- Dry mouth, no tears when crying
- Sunken eyes
- Sleepy, hard to wake
- Fast breathing or a fast heartbeat
Use a simple plan: small sips often. Large drinks can trigger more vomiting.
| GI Illness | Symptoms | Dehydration Signs | Duration | Oral Rehydration |
| Norovirus | Vomit + diarrhea | No tears, dry mouth | 24–48 hrs | Oral rehydration solution 1–2 oz/hr |
| Rotavirus | Severe watery diarrhea | Sunken soft spot (infants) | 5–7 days | 50 ml/kg first 4 hrs |
| Bacterial (Salmonella) | Bloody diarrhea, fever | Lethargy | ~7 days | Hospital if severe |
Rotavirus vaccine impact: Many children now avoid the worst cases because vaccination lowered severe illness and hospital visits in many communities.
Oral rehydration formula
- Weight (kg) x 50 ml = total in the first 4 hours
Then continue with small, steady amounts. If your child cannot keep any fluid down, call your pediatrician.
Food and drink tips
- Use an oral rehydration solution, not sports drinks
- Avoid juice, as it can worsen diarrhea
- Resume normal foods as tolerated; bland foods are fine
- Breastfeeding can continue
Skin Infections and Rashes
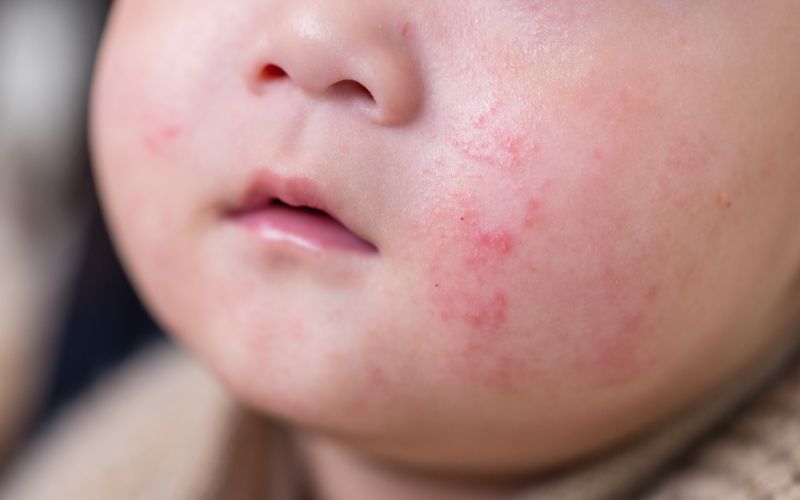
Rashes scare parents because they show up fast and can look dramatic. Many are viral and get better with time. Some are bacterial and need treatment. The key is to look at symptoms that come with the rash.
Here is a quick decision guide.
| Rash Type | Cause | Contagious | Treatment | School Rules |
| Hand-Foot-Mouth | Coxsackievirus | Yes, 7–10 days | Supportive care | Fever-free 24 hrs |
| Impetigo | Staph/Strep | Yes, until 24 hrs on antibiotics | Mupirocin or oral meds | 24 hrs on meds |
| Ringworm | Fungus | Yes, until treated | Antifungal cream | Cover lesions |
| Scarlet Fever | Strep | Yes, until 24 hrs on antibiotics | Antibiotics | Rash + fever improving |
Viral vs bacterial clues
- Viral rashes often come with a cold and mild fever, and the child still acts mostly normal.
- Bacterial rashes may crust, ooze, spread fast, or come with pain and higher fever.
Hand-foot-mouth tips
- The sore throat can be the worst part.
- Offer cold fluids, popsicles, and soft foods.
- Watch for dehydration if your child refuses to drink.
If a rash comes with trouble breathing, swelling of the lips, or if your child seems very weak, seek urgent care.
Vaccine-Preventable (Now Rare)
Some illnesses used to be common pediatric illnesses. Vaccines changed that. Many vaccine-preventable diseases are now unusual, but outbreaks can still happen, especially when a community has lower vaccination rates.
| Disease | Pre-Vaccine Annual Cases | Current Cases | Vaccine |
| Measles | 500,000 | < 100 | MMR |
| Chickenpox | 4 million | ~10,000 | Varicella |
| Rotavirus | 50,000 hospitalizations | Big reduction | Rotavirus vaccine |
Breakthrough infections can happen. If a vaccinated child gets one of these illnesses, it is often milder. Still, your child may need testing, isolation guidance, and close follow-up. If you think your child was exposed, call your pediatric office before you show up, so the team can plan safely.
Emerging Chronic Conditions
Today, many families manage chronic issues more than they manage rare vaccine-preventable diseases. These conditions can affect school, sports, sleep, mood, and long-term health. They also increase sick visits because symptoms flare during viral seasons.
Common issues families ask about include:
- ADHD: attention and behavior concerns at school and home
- Asthma: cough, wheeze, or breathing trouble that gets worse with colds
- Allergies: runny nose, itchy eyes, or skin flares
- Food allergies: hives, swelling, vomiting after certain foods
- Anxiety and depression in teens: sleep changes, mood shifts, school withdrawal. Addressing mental health early leads to better outcomes at school and at home
Many communities see these problems more often now. The best plan is steady care, clear follow-ups, and an action plan for flares. For asthma, that may mean knowing when to use a rescue inhaler and when symptoms require same-day care.
Richardson Seasonal Illness Calendar
Illness patterns change by season. Planning ahead can reduce stress, missed school days, and support your family’s health through every season.
| Month | Peak Illnesses | Local Surge |
| Aug/Sep | Back-to-school viral spread | ~30% visit increase |
| Nov–Feb | Flu and RSV season | After-hours care busiest |
| Apr–Jun | Allergies, strep | Sports injury peak |
What this means for families
- In late summer, focus on handwashing, sleep, and updated vaccines.
- In winter, watch breathing symptoms closely, especially for babies.
- In spring, know the difference between allergies and a cold.
When to Call Your Richardson Pediatrician for Your Sick Child
Use clear thresholds. If you are unsure, call. It is better to ask early than wait too long early action supports better health outcomes for your child.
Call the pediatrician the same day if:
- Fever in a baby under 3 months
- Breathing looks hard, fast, or noisy
- Cough with wheezing or chest pulling in
- Ear pain that is severe or not improving
- Vomiting that prevents keeping fluids down
- Signs of dehydration (no tears, very dry mouth, very low urine)
- Rash with fever that worries you, or rash that spreads fast
Go to urgent care or the ER if:
- Stridor at rest (harsh, noisy breathing in croup)
- Blue lips or face, or severe trouble breathing
- The child is very hard to wake or very confused
- Seizure, stiff neck, or severe headache
- Severe dehydration (very little urine, very weak, cannot drink)
If your child has a history of asthma, prematurity, or immune problems, call sooner. For guidance on whether to use the ER, you can also review the ER vs pediatrician in Richardson content on this site.
Frequently Asked Questions
What are the most common pediatric illnesses in young kids?
The most common pediatric illnesses include colds, ear infections, stomach bugs, and rashes. Most are viral and improve with home care.
How can I tell croup vs cold in kids?
A cold causes a runny nose and cough. Croup often causes a barking cough and noisy breathing, worse at night.
What are the symptoms of childhood illnesses that need urgent care?
Trouble breathing, dehydration, a fever in a baby under 3 months, or a child who is hard to wake should be checked right away.
How do I handle child stomach flu management at home?
Give small sips of oral rehydration solution often. Watch urine output and energy level. Call if your child cannot keep fluids down.
Home Management Toolkit
Keep a simple sick-day setup at home. It supports overall child health and makes common pediatric illnesses easier to manage.
Quick toolkit
- The thermometer you trust
- Oral rehydration solution
- Saline spray and bulb suction (for babies)
- Cool-mist humidifier
- Weight-based dosing chart for fever medicine
If you want help choosing the right visit type, see our book a pediatric appointment in Richardson and our pediatrician services in Richardson page.
